Health Library
Heart attack – discharge
Myocardial infarction - discharge; MI - discharge; Coronary event - discharge; Infarct - discharge; Acute coronary syndrome - discharge; ACS - discharge
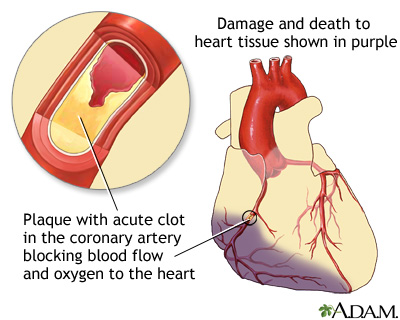
A heart attack occurs when blood flow to a part of your heart is blocked long enough that part of the heart muscle is damaged or dies. This article discusses what you need to do to take care of yourself after you leave the hospital.
Images
I Would Like to Learn About:
When You're in the Hospital
You were in the hospital because you had a heart attack. A heart attack occurs when blood flow to a part of your heart is blocked long enough that part of the heart muscle is damaged or dies.
What to Expect at Home
You may feel sad. You may feel anxious and as though you have to be very careful about what you do. All of these feelings are normal. They go away for most people after 2 or 3 weeks. You may also feel tired when you leave the hospital to go home.
Activity
You should know the signs and symptoms of angina.
- You may feel pressure, squeezing, burning, or tightness in your chest. You may also notice these symptoms in your arms, shoulders, neck, jaw, throat, or back.
- Some people also feel discomfort in their back, shoulders, and stomach area.
- You may have indigestion or feel sick to your stomach.
- You may feel tired and be short of breath, sweaty, lightheaded, or weak.
- You may have angina during physical activity, such as climbing stairs or walking uphill, lifting, sexual activity, or when you are out in cold weather. It can also happen when you are resting or it can wake you up when you are sleeping.
Know how to treat your chest pain when it happens. Talk with your health care provider about what to do.
Take it easy for the first 4 to 6 weeks after your heart attack.
- Avoid heavy lifting. Get some help with household chores if you can.
- Take 30 to 60 minutes to rest in the afternoon for first 4 to 6 weeks. Try to go to bed early and get plenty of sleep.
- Before starting to exercise, your provider may have you do an exercise test and recommend an exercise plan. This may happen before you leave the hospital or soon afterward. Do not change your exercise plan before talking with your provider.
- Your provider may refer you to cardiac rehabilitation program. There, you will learn how to slowly increase your exercise and how to take care of your heart disease.
You should be able to talk comfortably when you are doing any activity, such as walking, setting the table, and doing laundry. If you cannot, stop the activity.
Ask your provider about when you can return to work. Expect to be away from work for at least a week.
Talk to your provider before engaging in sexual activity. Ask your provider when it is OK to start again. Do not take Viagra, Levitra, Cialis or any herbal remedy for erection problems without checking with your provider first.
How long you will have to wait to return to your normal activities will depend on:
- Your physical condition before your heart attack
- The size of your heart attack
- If you had complications
- The overall speed of your recovery
Diet and Lifestyle
Do not drink any alcohol for at least 2 weeks. Ask your provider when you may start. Limit how much you drink. Women should have only 1 drink a day, and men should have no more than 2 a day. Try to drink alcohol only when you are eating.
If you smoke, stop. Ask your provider for help quitting if you need it. Do not let anybody smoke in your home, since second-hand smoke can harm you. Try to stay away from things that are stressful for you. If you are feeling stressed all the time, or if you are feeling very sad, talk with your provider. They can refer you to a counselor.
Learn more about what you should eat to make your heart and blood vessels healthier.
Taking Your Heart Medicines
Have your prescriptions filled before you go home. It is very important that you take your medicines the way your provider told you to. Do not take any other medicines or herbal supplements without asking your provider first if they are safe for you.
Take your medicines with water. Do not take them with grapefruit juice, since it may change how your body absorbs certain medicines. Ask your provider or pharmacist for more information about this.
The medicines below are given to most people after they have had a heart attack. Sometimes there is a reason they may not be safe to take, though. These medicines help prevent another heart attack. Talk with your provider if you are not already on any of these medicines:
- Antiplatelets medicines (blood thinners), such as aspirin, clopidogrel (Plavix), warfarin (Coumadin), prasugrel (Efient), or ticagrelor (Brilinta) to help keep your blood from clotting.
- Beta-blockers and ACE inhibitor medicines to help protect your heart.
- Statins or other drugs to lower your cholesterol.
Do not suddenly stop taking these medicines for your heart. Do not stop taking medicines for your diabetes, high blood pressure, or any other medical conditions you may have without talking with your provider first.
If you are taking a blood thinner such as warfarin (Coumadin), you may need to have extra blood tests on a regular basis to make sure your dose is correct.
When to Call the Doctor
Contact your provider if you feel:
- Pain, pressure, tightness, or heaviness in your chest, arm, neck, or jaw
- Shortness of breath
- Gas pains or indigestion
- Numbness in your arms
- Sweaty, or if you lose color
- Lightheaded
Changes in your angina may mean your heart disease is getting worse. Contact your provider if your angina:
- Becomes stronger
- Happens more often
- Lasts longer
- Occurs when you are not active or when you are resting
- Medicines do not help ease your symptoms as well as they used to
Related Information
Heart bypass surgeryAngioplasty and stent placement - carotid artery
Heart bypass surgery - minimally invasive
Ventricular assist device
Cardiac ablation procedures
Heart pacemaker
Implantable cardioverter-defibrillator
Heart attack
Unstable angina
High blood cholesterol levels
High blood pressure in adults - hypertension
Tips on how to quit smoking
Deep vein thrombosis - discharge
ACE inhibitors
Angina - when you have chest pain
Angina - discharge
Heart attack - discharge
Angioplasty and stent - heart - discharge
Aspirin and heart disease
Cholesterol - drug treatment
Being active when you have heart disease
Butter, margarine, and cooking oils
Cardiac catheterization - discharge
Heart pacemaker - discharge
Cholesterol and lifestyle
Antiplatelet drugs - P2Y12 inhibitors
Controlling your high blood pressure
Heart bypass surgery - discharge
Heart bypass surgery - minimally invasive - discharge
Dietary fats explained
Fast food tips
Heart disease - risk factors
How to read food labels
Implantable cardioverter defibrillator - discharge
Low-salt diet
Mediterranean diet
Being active after your heart attack
High blood pressure - what to ask your doctor
Heart attack - what to ask your doctor
Taking warfarin (Coumadin, Jantoven) - what to ask your doctor
Taking warfarin (Coumadin)
References
Amsterdam EA, Wenger NK, Brindis RG, et al. 2014 AHA/ACC guideline for the management of patients with non-ST-elevation acute coronary syndromes: a report of the American College of Cardiology/American Heart Association Task Force on practice guidelines. J Am Coll Cardiol. 2014;64(24):e139-e228. PMID: 25260718 pubmed.ncbi.nlm.nih.gov/25260718/.
Bohula EA, Morrow DA. ST-elevation myocardial infarction: management. In: Libby P, Bonow RO, Mann DL, Tomaselli GF, Bhatt DL, Solomon SD, eds. Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine. 12th ed. Philadelphia, PA: Elsevier; 2022:chap 38..
Fihn SD, Blankenship JC, Alexander KP, et al. 2014 ACC/AHA/AATS/PCNA/SCAI/STS focused update of the guideline for the diagnosis and management of patients with stable ischemic heart disease: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines, and the American Association for Thoracic Surgery, Preventive Cardiovascular Nurses Association, Society for Cardiovascular Angiography and Interventions, and Society of Thoracic Surgeons. J Thorac Cardiovasc Surg. 2015;149(3):e5-23. PMID: 25827388 pubmed.ncbi.nlm.nih.gov/25827388/.
Giugliano RP, Braunwald E. Non-ST elevation acute coronary syndromes. In: Libby P, Bonow RO, Mann DL, Tomaselli GF, Bhatt DL, Solomon SD, eds. Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine. 12th ed. Philadelphia, PA: Elsevier; 2022:chap 39.
Kumbhani DJ, Bhatt DL. Percutaneous coronary intervention. In: Libby P, Bonow RO, Mann DL, Tomaselli GF, Bhatt DL, Solomon SD, eds. Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine. 12th ed. Philadelphia, PA: Elsevier; 2022:chap 41.
Morrow DA, de Lemos J. Stable ischemic heart disease. In: Libby P, Bonow RO, Mann DL, Tomaselli GF, Bhatt DL, Solomon SD, eds. Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine. 12th ed. Philadelphia, PA: Elsevier; 2022:chap 40.
O'Gara PT, Kushner FG, Ascheim DD, et al. 2013 ACCF/AHA guideline for the management of ST-elevation myocardial infarction: executive summary: a report of the American College of Cardiology Foundation/American Heart Association Task Force on practice guidelines. Circulation. 2013;127(4):529-555. PMID: 23247303 pubmed.ncbi.nlm.nih.gov/23247303/.
BACK TO TOPReview Date: 8/16/2022
Reviewed By: Michael A. Chen, MD, PhD, Associate Professor of Medicine, Division of Cardiology, Harborview Medical Center, University of Washington Medical School, Seattle, WA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.
 | A.D.A.M., Inc. is accredited by URAC, for Health Content Provider (www.urac.org). URAC's accreditation program is an independent audit to verify that A.D.A.M. follows rigorous standards of quality and accountability. A.D.A.M. is among the first to achieve this important distinction for online health information and services. Learn more about A.D.A.M.'s editorial policy, editorial process and privacy policy. A.D.A.M. is also a founding member of Hi-Ethics. This site complies with the HONcode standard for trustworthy health information: verify here. |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. © 1997- 2022 A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited.
