Health Library
Heart attack
Myocardial infarction; MI; Acute MI; ST-elevation myocardial infarction; Non-ST-elevation myocardial infarction; NSTEMI; CAD - heart attack; Coronary artery disease - heart attack
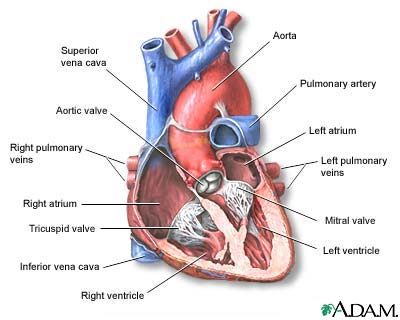
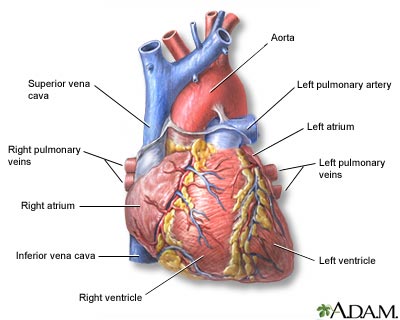
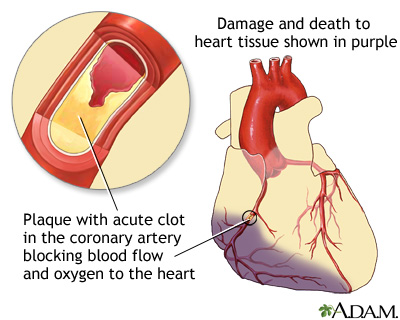
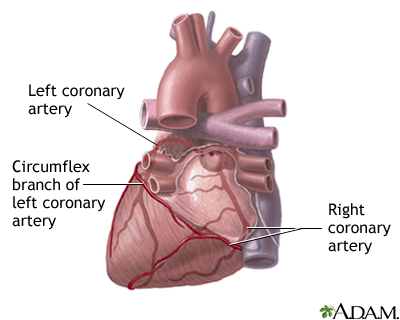
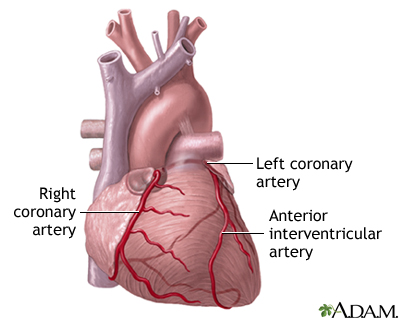
Most heart attacks are caused by a blood clot that blocks one of the coronary arteries. The coronary arteries bring blood and oxygen to the heart. If the blood flow is blocked, the heart is starved of oxygen and heart cells die.
The medical term for this is myocardial infarction.
Images
I Would Like to Learn About:
Causes
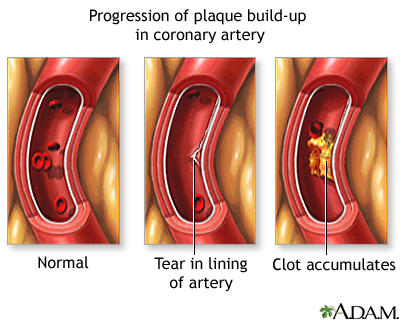
A substance called plaque can build up in the walls of your coronary arteries. This plaque is made up of cholesterol and other cells.
A heart attack may occur when:
- A disruption in the plaque occurs. This triggers blood platelets and other substances to form a blood clot at the site that blocks most or all of the oxygen-carrying blood from flowing to a part of the heart muscle. This is the most common cause of heart attack.
The cause of heart attack is not always known, but there are well known risk factors.
Heart attack may occur:
- When you are resting or asleep
- After a sudden increase in physical activity
- When you are active outside in cold weather
- After sudden, severe emotional or physical stress, including an illness
Many risk factors may lead to the development of plaque buildup and a heart attack.
Symptoms
A heart attack is a medical emergency. If you have symptoms of a heart attack, call 911 or your local emergency number right away.
- DO NOT try to drive yourself to the hospital.
- DO NOT WAIT. You are at greatest risk for sudden death in the early hours of a heart attack.
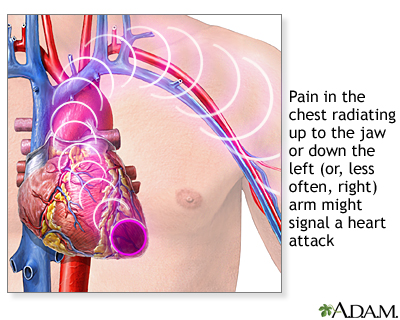
Chest pain is the most common symptom of a heart attack.
- You may feel the pain in only one part of your body OR
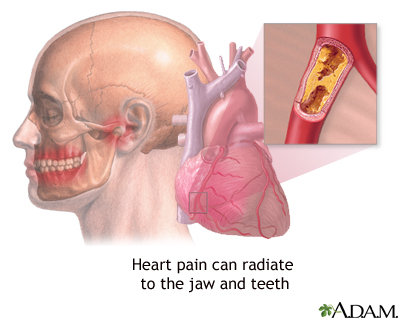
- Pain may move from your chest to your arms, shoulder, neck, teeth, jaw, belly area, or back
The pain can be severe or mild. It can feel like:
- A tight band around the chest
- Bad indigestion
- Something heavy sitting on your chest
- Squeezing or heavy pressure
The pain most often lasts longer than 20 minutes. Rest and a medicine to relax the blood vessels (called nitroglycerin) may not completely relieve the pain of a heart attack. Symptoms may also go away and come back.
Other symptoms of a heart attack can include:
- Anxiety
- Cough
- Fainting
- Lightheadedness, dizziness
- Nausea and vomiting
- Palpitations (feeling like your heart is beating too fast or irregularly)
- Shortness of breath
- Sweating, which may be very heavy
Some people (including older adults, people with diabetes, and women) may have little or no chest pain. Or, they may have atypical symptoms such as shortness of breath, fatigue, and weakness. A "silent heart attack," which can also occur, is a heart attack with no symptoms.
Exams and Tests
A health care provider will perform a physical exam and listen to your chest using a stethoscope.
- The provider may hear abnormal sounds in your lungs (called crackles), a heart murmur, or other abnormal sounds.
- You may have a fast or uneven pulse.
- Your blood pressure may be normal, high, or low.
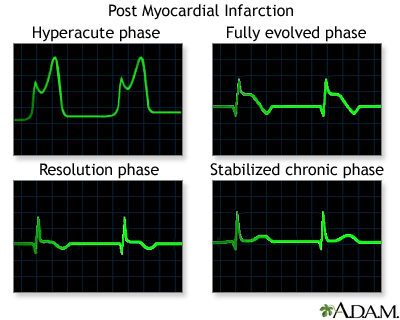
You will have an electrocardiogram (ECG) to look for heart damage. Often, certain changes on the ECG indicate you are having a heart attack, although a heart attack can also occur without ECG changes.
A blood test can show if you have heart tissue damage. This test can confirm that you are having a heart attack. The test is often repeated over time.
Coronary angiography may be done right away or later in the course of illness.
- This test uses a special dye and x-rays to see how blood flows through your heart.
- It can help your provider decide which treatments you need next.
Other tests to look at your heart that may be done while you are in the hospital:
- Echocardiography with or with stress testing
- Exercise stress test
- Nuclear stress test
- Heart CT scan or heart MRI
Treatment
IMMEDIATE TREATMENT
- You will be hooked up to a heart monitor, so the health care team can see how regularly your heart is beating.
- You will receive oxygen.
- An intravenous line (IV) will be placed into one of your veins. Medicines and fluids pass through this IV.
- You may get nitroglycerin and morphine to help reduce chest pain.
- You may receive aspirin, unless it would not be safe for you. In that case, you will be given another medicine that prevents blood clots.
- Dangerous abnormal heartbeats (arrhythmias) may be treated with medicine or electric shocks.
EMERGENCY PROCEDURES
Angioplasty is a procedure to open narrowed or blocked blood vessels that supply blood to the heart.
- Angioplasty is often the first choice of treatment. It should be done within 90 minutes after you get to the hospital, and usually no later than 12 hours after a heart attack.
- A stent is a small, metal mesh tube that opens up (expands) inside a coronary artery. A stent is usually placed after or during angioplasty. It helps prevent the artery from closing up again.
You may be given drugs to break up the clot. This is called thrombolytic therapy. It is best if these drugs are given soon after the onset of symptoms, usually no later than 12 hours after it and ideally within 30 minutes of arriving at the hospital.
Some people may also have heart bypass surgery to open narrowed or blocked blood vessels that supply blood to the heart. This procedure is also called coronary artery bypass grafting or open heart surgery.
TREATMENT AFTER A HEART ATTACK
After several days, you will be discharged from the hospital.
You will likely need to take medicines, some for the rest of your life. Always talk to your provider before stopping or changing how you take any medicines. Stopping certain medicines can be deadly.
While under the care of your health care team, you will learn:
- How to take medicines to treat your heart problem and prevent more heart attacks
- How to eat a heart-healthy diet
- How to be active and exercise safely
- What to do when you have chest pain
- How to stop smoking
Strong emotions are common after a heart attack.
- You may feel sad
- You may feel anxious and worry about being careful about everything you do
All of these feelings are normal. They go away for most people after 2 or 3 weeks.
You may also feel tired when you leave the hospital to go home.
Most people who have had a heart attack take part in a cardiac rehabilitation program.
Support Groups
Many people benefit from taking part in support groups for people with heart disease.
Outlook (Prognosis)
After a heart attack, you have a higher chance of having another heart attack.
How well you do after a heart attack depends on several factors such as:
- The amount of damage to your heart muscle and heart valves
- Where that damage is located
- Your medical care after the heart attack
If your heart can no longer pump blood out to your body as well as it used to, you may develop heart failure. Abnormal heart rhythms can occur, and they can be life threatening.
Most people can slowly go back to normal activities after a heart attack. This includes sexual activity. Talk to your provider about how much activity is good for you.
Related Information
AtherosclerosisStress and your health
Risks of tobacco
High blood pressure in adults - hypertension
Diabetes
Arrhythmias
Ventricular tachycardia
Heart failure
Cardiogenic shock
Pericarditis
Lipoprotein-a
Metabolic syndrome
Implantable cardioverter-defibrillator
Cholesterol - what to ask your doctor
Heart failure - what to ask your doctor
High blood pressure - what to ask your doctor
Heart attack - what to ask your doctor
Taking warfarin (Coumadin, Jantoven) - what to ask your doctor
Taking warfarin (Coumadin)
Cholesterol - drug treatment
Heart attack - discharge
Angioplasty and stent - heart - discharge
References
Amsterdam EA, Wenger NK, Brindis RG, et al. 2014 AHA/ACC guideline for the management of patients with non-ST-elevation acute coronary syndromes: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. J Am Coll Cardiol. 2014;64(24):e139-e228. PMID: 25260718 pubmed.ncbi.nlm.nih.gov/25260718/.
Arnett DK, Blumenthal RS, Albert MA, et al. 2019 ACC/AHA guideline on the primary prevention of cardiovascular disease: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. Circulation. 2019;140(11):e596-e646. PMID: 30879355 pubmed.ncbi.nlm.nih.gov/30879355/.
Bohula EA, Morrow DA. ST-elevation myocardial infarction: management. In: Libby P, Bonow RO, Mann DL, Tomaselli GF, Bhatt DL, Solomon SD, eds. Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine. 12th ed. Philadelphia, PA: Elsevier; 2022:chap 38.
Giugliano RP, Braunwald E. Non-ST elevation acute coronary syndromes. In: Libby P, Bonow RO, Mann DL, Tomaselli, GF, Bhatt DL, Solomon SD, eds. Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine. 12th ed. Philadelphia, PA: Elsevier; 2022:chap 39.
O'Gara PT, Kushner FG, Ascheim DD, et al. 2013 ACCF/AHA guideline for the management of ST-elevation myocardial infarction: a report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines. J Am Coll Cardiol. 2013;61(4):485-510. PMID: 23256913 pubmed.ncbi.nlm.nih.gov/23256913/.
Scirica BM, Libby P, Morrow DA. ST-elevation myocardial infarction: pathophysiology and clinical evolution. In: Libby P, Bonow RO, Mann DL, Tomaselli GF, Bhatt DL, Solomon SD, eds. Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine. 12th ed. Philadelphia, PA: Elsevier; 2022:chap 37.
Tamis-Holland JE, Jneid H, Reynolds HR, et al. Contemporary diagnosis and management of patients with myocardial infarction in the absence of obstructive coronary artery disease: a scientific statement from the American Heart Association. Circulation. 2019;139(18):e891-e908. PMID: 30913893 pubmed.ncbi.nlm.nih.gov/30913893/.
BACK TO TOPReview Date: 10/5/2022
Reviewed By: Thomas S. Metkus, MD, Assistant Professor of Medicine and Surgery, Johns Hopkins University School of Medicine, Baltimore, MD. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.
 | A.D.A.M., Inc. is accredited by URAC, for Health Content Provider (www.urac.org). URAC's accreditation program is an independent audit to verify that A.D.A.M. follows rigorous standards of quality and accountability. A.D.A.M. is among the first to achieve this important distinction for online health information and services. Learn more about A.D.A.M.'s editorial policy, editorial process and privacy policy. A.D.A.M. is also a founding member of Hi-Ethics. This site complies with the HONcode standard for trustworthy health information: verify here. |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. © 1997- 2022 A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited.
