Health Library
Controlling your high blood pressure
Controlling hypertension
Images

I Would Like to Learn About:
Description
Hypertension is another term used to describe high blood pressure. High blood pressure can lead to:
You are more likely to have high blood pressure as you get older. This is because your blood vessels become stiffer as you age. When that happens, your blood pressure goes up.
When is Your Blood Pressure a Concern?
If your blood pressure is high, you need to lower it and keep it under control. Your blood pressure reading has 2 numbers. One or both of these numbers can be too high.
- The top number is called the systolic blood pressure. For most people, this reading is too high if it is 140 or higher.
- The bottom number is called the diastolic blood pressure. For most people, this reading is too high if it is 90 or higher.
The above blood pressure numbers are goals that most experts agree on for most people. For some people age 60 years and above, some health care providers recommend a blood pressure goal of 150/90. Some patients may have blood pressure goals lower than these targets, in particular circumstances. Your provider will work with you to create a blood pressure goal that applies to you specifically.
Medicines for Blood Pressure
Many medicines can help you control your blood pressure. Your provider will:
- Prescribe the best medicine for you
- Monitor your medicines
- Make changes if needed
Older adults tend to take more medicines and this puts them at greater risk for harmful side effects. One side effect of blood pressure medicine is an increased risk for falls. When treating older adults, blood pressure goals need to be balanced against medicine side effects.
Diet, Exercise, and Other Lifestyle Changes
In addition to taking medicine, you can do many things to help control your blood pressure. Some of these include:
- Limit the amount of sodium (salt) you eat. Aim for less than 1,500 mg per day.
- Limit how much alcohol you drink, no more than 1 drink a day for women and 2 a day for men.
- Eat a heart-healthy diet that includes the recommended amounts of potassium and fiber.
- Drink plenty of water.
- Stay at a healthy body weight. Find a weight-loss program, if you need it.
- Exercise regularly. Get at least 40 minutes of moderate to vigorous aerobic exercise at least 3 to 4 days a week aiming for at least 150 minutes per week.
- Reduce stress. Try to avoid things that cause you stress, and try meditation or yoga to de-stress.
- If you smoke, quit. Find a program that will help you stop.
Your provider can help you find programs for losing weight, stopping smoking, and exercising. You can also get a referral to a dietitian from your provider. The dietitian can help you plan a diet that is healthy for you.
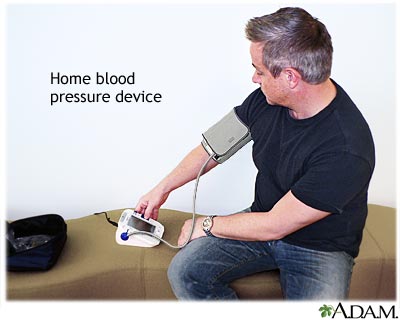
Checking Your Blood Pressure
Your blood pressure can be measured at many places, including:
- Home
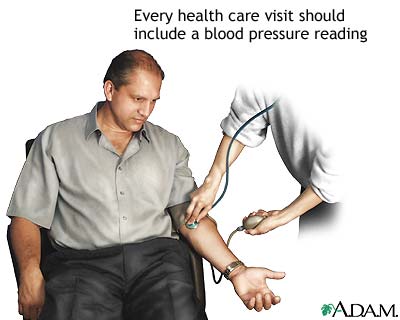
- Your provider's office
- Your local fire station
- Some pharmacies
Your provider may ask you to keep track of your blood pressure at home. Make sure you get a good quality, well-fitting home device. It is best to have one with a cuff for your arm and a digital readout. Practice with your provider to make sure you are taking your blood pressure correctly.
It is normal for your blood pressure to be different at different times of the day.
It is most often higher when you are at work. It drops slightly when you are at home. It is most often lowest when you are sleeping.
It is normal for your blood pressure to increase suddenly when you wake up. For people with very high blood pressure, this is when they are most at risk for heart attack and stroke.
Follow-up
Your provider will give you a physical exam and check your blood pressure often. With your provider, establish a goal for your blood pressure.
If you monitor your blood pressure at home, keep a written record. Bring the results to your clinic visit.
When to Call the Doctor
Contact your provider if your blood pressure goes well above your normal range.
Also contact your provider if you have any of the following symptoms:
- Severe headache
- Irregular heartbeat or pulse
- Chest pain
- Sweating
- Nausea or vomiting
- Shortness of breath
- Dizziness or lightheadedness
- Pain or tingling in the neck, jaw, shoulder, or arms
- Numbness or weakness in your body
- Fainting
- Trouble seeing
- Confusion
- Difficulty speaking
- Other side effects that you think might be from your medicine or your blood pressure
Related Information
Heart bypass surgeryCarotid artery surgery - open
Angioplasty and stent placement - carotid artery
Heart bypass surgery - minimally invasive
Cardiac ablation procedures
Heart pacemaker
Implantable cardioverter-defibrillator
Heart failure
High blood cholesterol levels
High blood pressure in adults - hypertension
Angina
Coronary heart disease
Tips on how to quit smoking
Angioplasty and stent placement - peripheral arteries
Peripheral artery bypass - leg
ACE inhibitors
Angina - discharge
Heart attack – discharge
Angioplasty and stent - heart - discharge
Aspirin and heart disease
Being active when you have heart disease
Butter, margarine, and cooking oils
Cholesterol and lifestyle
Heart bypass surgery - discharge
Heart bypass surgery - minimally invasive - discharge
Dietary fats explained
Fast food tips
Heart disease - risk factors
How to read food labels
Low-salt diet
Mediterranean diet
Heart failure - fluids and diuretics
Heart failure - home monitoring
Heart failure - discharge
Stroke - discharge
Diabetes - preventing heart attack and stroke
Antiplatelet drugs - P2Y12 inhibitors
High blood pressure - what to ask your doctor
Angioplasty and stent placement - peripheral arteries - discharge
Angioplasty and stent placement - carotid artery - discharge
Aortic aneurysm repair - endovascular - discharge
Atrial fibrillation - discharge
Carotid artery surgery - discharge
Peripheral artery bypass - leg - discharge
Abdominal aortic aneurysm repair - open - discharge
Cholesterol - drug treatment
References
American Diabetes Association Professional Practice Committee. 10. Cardiovascular disease and risk management: standards of medical care in diabetes-2022. Diabetes Care. 2022;45(9):2178-2181. PMID: 34964815 pubmed.ncbi.nlm.nih.gov/34964815/.
Bakris GL, Sorrentino MJ. Systemic hypertension: mechanisms, diagnosis, and treatment. In: Libby P, Bonow RO, Mann DL, Tomaselli GF, Bhatt DL, Solomon SD, eds. Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine. 12th ed. Philadelphia, PA: Elsevier; 2022:chap 26.
Ettehad D, Emdin CA, Kiran A, et al. Blood pressure lowering for prevention of cardiovascular disease and death: a systematic review and meta-analysis. Lancet. 2016;387(10022):957-967. PMID: 26724178 pubmed.ncbi.nlm.nih.gov/26724178/.
Rosendorff C, Lackland DT, Allison M, et al. Treatment of hypertension in patients with coronary artery disease: a scientific statement from the American Heart Association, American College of Cardiology, and American Society of Hypertension. Circulation. 2015;131(19):e435-e470. PMID: 25829340 pubmed.ncbi.nlm.nih.gov/25829340/.
Whelton PK, Carey RM, Aronow WS, et al. ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA guideline for the prevention, detection, evaluation, and management of high blood pressure in adults: a report of the American College of Cardiology/American Heart Association Task Force on clinical practice guidelines. J Am Coll Cardiol. 2018;72(3):e33. PMID: 29133354 pubmed.ncbi.nlm.nih.gov/29133354/.
BACK TO TOPReview Date: 8/23/2022
Reviewed By: Thomas S. Metkus, MD, Assistant Professor of Medicine and Surgery, Johns Hopkins University School of Medicine, Baltimore, MD. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.
 | A.D.A.M., Inc. is accredited by URAC, for Health Content Provider (www.urac.org). URAC's accreditation program is an independent audit to verify that A.D.A.M. follows rigorous standards of quality and accountability. A.D.A.M. is among the first to achieve this important distinction for online health information and services. Learn more about A.D.A.M.'s editorial policy, editorial process and privacy policy. A.D.A.M. is also a founding member of Hi-Ethics. This site complies with the HONcode standard for trustworthy health information: verify here. |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. © 1997- 2023 A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited.
