Pericarditis - after heart attack
Dressler syndrome; Post-MI pericarditis; Post-cardiac injury syndrome; Postcardiotomy pericarditis
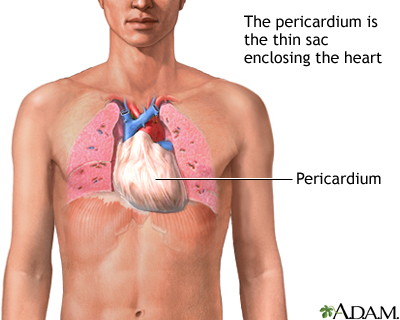
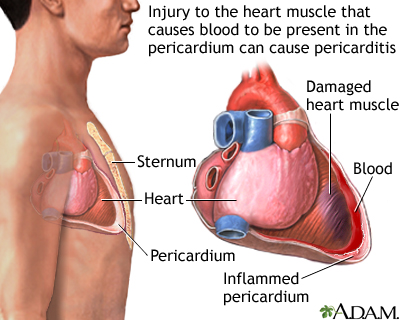
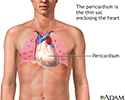
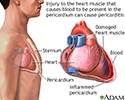
Pericarditis is inflammation and swelling of the covering of the heart (pericardium). It can occur in the days or weeks following a heart attack.
Causes
Two types of pericarditis can occur after a heart attack.
Early pericarditis: This form most often occurs within 1 to 3 days after a heart attack. Inflammation and swelling develop as the body tries to clean up the damaged heart tissue.
Late pericarditis: This is also called Dressler syndrome. It is also called post-cardiac injury syndrome or postcardiotomy pericarditis). It most often develops several weeks or months after a heart attack, heart surgery, or other trauma to the heart. It can also happen a week after a heart injury. Dressler syndrome is thought to occur when the immune system attacks healthy heart tissue by mistake.
Things that put you at higher risk for pericarditis include:
- A previous heart attack
- Open heart surgery
- Chest trauma
- A heart attack that has affected the thickness of your heart muscle
Symptoms
Symptoms include:
- Anxiety
- Chest pain from the swollen pericardium rubbing on the heart. The pain may be sharp, tight or crushing and may move to the neck, shoulder, or abdomen. The pain may also be worse when you breathe and go away when you lean forward, stand, or sit up.
- Trouble breathing
- Dry cough
- Fast heart rate (tachycardia)
- Fatigue
- Fever (common with the second type of pericarditis)
- Malaise (general ill feeling)
- Splinting of ribs (bending over or holding the chest) with deep breathing
Exams and Tests
The health care provider will listen to your heart and lungs with a stethoscope. There may be a rubbing sound (called a pericardial friction rub, not to be confused with a heart murmur). Heart sounds in general may be weak or sound far away.
A buildup of fluid in the covering of the heart or space around the lungs (pericardial effusion) is not common after a heart attack. But, it often does occur in some people with Dressler syndrome.
Tests may include:
- Cardiac injury markers (CK-MB and troponin may help tell pericarditis from a heart attack)
- Chest CT scan
- Chest MRI
- Chest x-ray
- Complete blood count (CBC)
- ECG (electrocardiogram)
- Echocardiogram
- ESR (sedimentation rate) or C-reactive protein (measures of inflammation)
Treatment
The goal of treatment is to make the heart work better and reduce pain and other symptoms.
Aspirin may be used to treat inflammation of the pericardium. A drug called colchicine is often used as well.
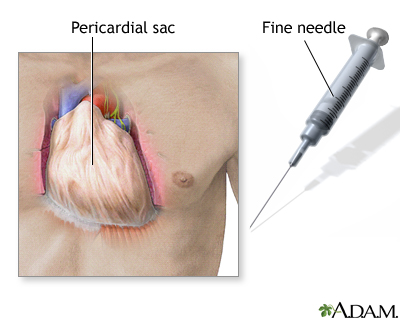
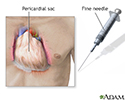
In some cases, excess fluid surrounding the heart (pericardial effusion) may need to be removed. This is done with a procedure called pericardiocentesis. If complications develop, part of the pericardium may sometimes need to be removed with surgery (pericardiectomy).
Outlook (Prognosis)
The condition may recur in some cases.
Possible Complications
Possible complications of pericarditis are:
When to Contact a Medical Professional
Contact your provider if:
- You develop symptoms of pericarditis after a heart attack
- You have been diagnosed with pericarditis and symptoms continue or come back despite treatment
References
Jouriles NJ. Pericardial and myocardial disease. In: Libby P, Bonow RO, Mann DL, Tomaselli, GF, Bhatt DL, Solomon SD, eds. Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine. 12th ed. Philadelphia, PA: Elsevier; 2022:chap 68.
Lewinter MM, Cremer PC, Klein AL. Pericardial diseases. In: Libby P, Bonow RO, Mann DL, Tomaselli, GF, Bhatt DL, Solomon SD, eds. Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine. 12th ed. Philadelphia, PA: Elsevier; 2022:chap 86.
Maisch B, Ristic AD. Pericardial diseases. In: Vincent J-L, Abraham E, Moore FA, Kochanek PM, Fink MP, eds. Textbook of Critical Care. 7th ed. Philadelphia, PA: Elsevier; 2017:chap 84.
Acute MI - illustration
Acute MI
illustration
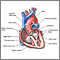
Pericardium - illustration
Pericardium
illustration
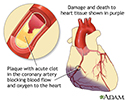
Pericarditis post-IM - illustration
Pericarditis post-IM
illustration
Pericardium - illustration
Pericardium
illustration
Review Date: 10/5/2022
Reviewed By: Thomas S. Metkus, MD, Assistant Professor of Medicine and Surgery, Johns Hopkins University School of Medicine, Baltimore, MD. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.