High blood sugar - self-care
Hyperglycemia - self care; High blood glucose - self care; Diabetes - high blood sugar
High blood sugar is also called high blood glucose, or hyperglycemia.
High blood sugar almost always happens in people who have diabetes. High blood sugar occurs when:
- Your body makes too little insulin.
- Your body does not respond to the signal insulin is sending.
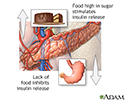
Insulin is a hormone that helps the body move glucose (sugar) from the blood into muscle or fat, where it is stored for later use when energy is needed.
Sometimes high blood sugar occurs due to stress from surgery, infection, trauma, or medicines. After the stress is over, blood sugar returns to normal.
Symptoms of High Blood Sugar
Symptoms of high blood sugar can include:
- Being very thirsty or having a dry mouth
- Having blurry vision
- Having dry skin
- Feeling weak or tired
- Needing to urinate a lot, or needing to get up more often than usual at night to urinate
You may have other, more serious symptoms if your blood sugar becomes very high or remains high for a long time. Over time, high blood sugar weakens your immune system and makes it more likely for you to get infections.
What to Think About When Your Blood Sugar is High
High blood sugar can harm you. If your blood sugar is high, you need to know how to bring it down. If you have diabetes, here are some questions to ask yourself when your blood sugar is high:
- Are you eating right?
- Are you eating too much?
- Have you been following your diabetes meal plan?
- Did you have a meal or a snack with a lot of carbohydrates, starches, or simple sugars?
Are you taking your diabetes medicines correctly?
- Has your doctor changed your medicines?
- If you take insulin, have you been taking the correct dose? Is the insulin expired? Or has it been stored in a hot or cold place?
- Are you afraid of having low blood sugar? Is that causing you to eat too much or take too little insulin or other diabetes medicine?
- Have you injected insulin into a scar or overused area? Have you been rotating sites? Was the injection into a lump or numb spot under the skin?
What else has changed?
- Have you been less active than usual?
- Do you have a fever, cold, flu, or another illness?
- Are you dehydrated?
- Have you had some stress?
- Have you been checking your blood sugar regularly?
- Have you gained weight?
- Have you started taking any new medicines such as for high blood pressure or other medical problems?
- Have you had an injection into a joint or other area with a glucocorticoid medicine?
Preventing High Blood Sugar
To prevent high blood sugar, you will need to:
- Follow your meal plan
- Stay physically active
- Take your diabetes medicines as instructed
You and your doctor will:
- Set a target goal for your blood sugar levels for different times during the day. This helps you manage your blood sugar.
- Decide how often you need to check your blood sugar at home.
If your blood sugar is higher than your goals over 3 days and you don't know why, check your urine for ketones. Then call your health care provider.
References
American Diabetes Association Professional Practice Committee. 5. Facilitating Behavior Change and Well-being to Improve Health Outcomes: Standards of Medical Care in Diabetes-2022. Diabetes Care. 2022;45(Suppl 1):S60-S82. PMID: 34964866 pubmed.ncbi.nlm.nih.gov/34964866/.
American Diabetes Association Professional Practice Committee. 6. Glycemic Targets: Standards of Medical Care in Diabetes-2022. Diabetes Care. 2022;45(Suppl 1):S83-S96. PMID: 34964868 pubmed.ncbi.nlm.nih.gov/34964868/.
Atkinson MA, Mcgill DE, Dassau E, Laffel L. Type 1 diabetes. In: Melmed S, Auchus RJ, Goldfine AB, Koenig RJ, Rosen CJ, eds. Williams Textbook of Endocrinology. 14th ed. Philadelphia, PA: Elsevier; 2020:chap 36.
Riddle MC, Ahmann AJ. Therapeutics of type 2 diabetes. In: Melmed S, Auchus RJ, Goldfine AB, Koenig RJ, Rosen CJ, eds. Williams Textbook of Endocrinology. 14th ed. Philadelphia, PA: Elsevier; 2020:chap 35.
- High blood sugar - self-care
- Low blood sugar - self-care
- Type 2 diabetes - self-care
- Gestational diabetes - self-care
- Venous ulcers - self-care
- Ischemic ulcers - self-care
- Peripheral artery disease of the legs - self-care
- Carotid artery stenosis - self-care
- Nerve damage from diabetes - self-care
- Vaginitis - self-care
Review Date: 2/1/2022
Reviewed By: Sandeep K. Dhaliwal, MD, board-certified in Diabetes, Endocrinology, and Metabolism, Springfield, VA. Also reviewed by David Zieve, MD, MHA, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.