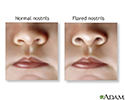
Nasal flaring
Flaring of the alae nasi (nostrils); Nostrils - flaring
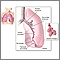
Nasal flaring occurs when the nostrils widen while breathing. It is often a sign of trouble breathing.
Considerations
Nasal flaring is seen mostly in infants and younger children.
Any condition that causes difficulty breathing can cause nasal flaring. Many causes of nasal flaring are not serious, but some can be life threatening.
In young infants, nasal flaring can be a sign of respiratory distress. This is a serious lung condition that prevents enough oxygen from getting to the lungs and into the blood.
Causes
Nasal flaring may be caused by any of the following:
- Asthma flare-up
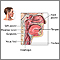
- Blocked airway (any cause)
- Swelling and mucus buildup in the smallest air passages in the lungs (bronchiolitis)
- Problem breathing and a barking cough (croup)
- Swollen or inflamed tissue in the area that covers the windpipe (epiglottitis)
- Lung problems, such as infection or long-term damage
- Breathing disorder in newborns (transient tachypnea of the newborn)
Home Care
Seek emergency help right away if you or your child has signs of a breathing difficulty.
When to Contact a Medical Professional
Call your health care provider if:
- There is any persistent, unexplained nasal flaring, especially in a young child.
- Bluish color develops in the lips, nail beds, or skin. This is a sign that breathing difficulty is severe. It may mean that an emergency condition is developing.
- You think that your child is having trouble breathing.
What to Expect at Your Office Visit
The provider will perform a physical exam and ask about the symptoms and medical history. Questions may include:
- When did the symptoms start?
- Are they getting better or worse?
- Is the breathing noisy, or are there wheezing sounds?
- What other symptoms are there, such as sweating or feeling tired?
- Do the muscles of the stomach, shoulders, or rib cage pull inward during breathing?
The provider will listen carefully to the breath sounds. This is called auscultation.
Tests that may be done include:
- Arterial blood gas analysis
- Complete blood count (CBC)
- ECG to check the heart
- Pulse oximetry to measure blood oxygen level
- X-rays of the chest
Oxygen may be given if there is a breathing problem.
References
Rodrigues KK. Roosevelt GE. Acute inflammatory upper airway obstruction (croup, epiglottitis, laryngitis, and bacterial tracheitis). In: Kliegman RM, St. Geme JW, Blum NJ, Shah SS, Tasker RC, Wilson KM, eds. Nelson Textbook of Pediatrics. 21st ed. Philadelphia, PA: Elsevier; 2020:chap 412.
Sarnaik AP, Clark JA, Heidemann SM. Respiratory distress and failure. In: Kliegman RM, St. Geme JW, Blum NJ, Shah SS, Tasker RC, Wilson KM, eds. Nelson Textbook of Pediatrics. 21st ed. Philadelphia, PA: Elsevier; 2020:chap 89.
Review Date: 6/7/2022
Reviewed By: Neil K. Kaneshiro, MD, MHA, Clinical Professor of Pediatrics, University of Washington School of Medicine, Seattle, WA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.