Which Colorectal Cancer Screening is Best for You?
posted on: 3/21/2019 12:57:20 PM
Shannon Wesley, DO
Midwest Surgical Specialists
Lima Memorial Physicians

Most patients see their primary care providers for annual well visits. If you are someone who does not have a primary care provider, my first advice to you is to please find a provider you trust and to begin seeing them regularly. People who are proactive in their care have grown accustomed to routine blood draws and urine tests. Women get yearly Pap smears and mammograms, while men get digital rectal exams. More recently, providers have joined the United States Preventive Services Task Force (USPSTF) to adapt further recommendations on which routine screening tests should be completed. Colorectal cancer screenings are now widely talked about during a patient’s well visit. Screening for colon cancer typically begins at the age of 50, however, last year the American Cancer Society changed the recommendation to age 45. Patients typically do not discuss their colon health with their physician until around this age, unless they are symptomatic. If there is family history of colon cancer, colon polyps or if an individual develops symptoms, testing may be recommended at an earlier age.
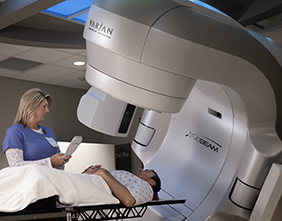
The most reliable screening tool for early detection is a colonoscopy. During this outpatient procedure, physicians are able to see inside the colon and identify problems including colon polyps. Most colorectal cancers begin as a polyp; a growth in the tissue of the colon or rectum. Colon polyps are various shapes and sizes, and they may be flat or raised. Polyps are common in people older than 50 years of age, and most are benign. There are certain types of polyps that have a higher risk of developing into cancer. Currently, a colonoscopy is the only test that allows physicians to identify and remove these colon polyps before they have the ability to become cancerous.
There are various situations when a colonoscopy may not be appropriate. In these situations, other tests can be performed to screen for problems that may lead to colorectal cancer. This can include testing stool for blood or DNA to determine a patient’s individual risk for colon cancer. Fecal immunochemical test (FIT) or guaiac-based fecal occult blood test (gFOBT) are simple tests that can detect blood in the stool and are done in the privacy of one’s own home. It is important to note benign and cancerous polyps do not bleed continuously. As a result, occult blood tests must be done on several stool samples and repeated yearly. The most common DNA stool test on the market currently is called Cologuard. Cologuard is an easy to use, noninvasive colon cancer screening test that can also be performed at home. It identifies altered DNA in stool, which can be associated with the possibility of colon cancer or pre-cancer. Cologuard is recommended to be performed every three years. Radiological imaging (double-contrast barium enema or a computed tomography colonography) are also tools that may be used to identify abnormalities in the colon or rectum. Images of the colon are produced via x-rays and computerized for analysis. To provide the best results, this test requires interpretation by a skilled radiologist, and is recommended every five years.
There is no single “best test” for any person; each test has its pros and cons. You should talk to your doctor at your next well visit about the advantages and disadvantages each test has to offer you. The screening test you choose depends on a combination of your preferences, medical condition, family history and likeliness to complete the test. The best screening for colon cancer is always the one that is being done!

Sources
American Cancer Society
American Society of Clinical Oncology
Centers for Disease Control & Prevention
U.S. Preventive Services Task Force
Originally published in The Lima News Health and Fitness section.
Website