RBC count
Erythrocyte count; Red blood cell count; Anemia - RBC count
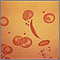
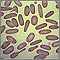
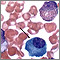
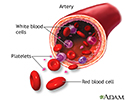
An RBC count is a blood test that measures how many red blood cells (RBCs) you have.
RBCs contain hemoglobin, a protein which carries oxygen. How much oxygen your body tissues get depends on how many RBCs you have and how well they work.
How the Test is Performed
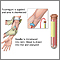
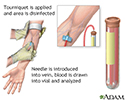
A blood sample is needed.
How to Prepare for the Test
No special preparation is necessary.
How the Test will Feel
When the needle is inserted to draw blood, some people feel moderate pain. Others feel only a prick or stinging. Afterward, there may be some throbbing or a slight bruise. This soon goes away.
Why the Test is Performed
The RBC count is almost always part of a complete blood count (CBC) test.
The test can help diagnose different kinds of anemia (low number of RBCs) and other conditions affecting red blood cells.
Other conditions that may require an RBC count are:
- Bone marrow disorder in which the marrow is replaced by scar tissue (myelofibrosis)
- Disease that damages kidney blood vessels (Alport syndrome)
- Disorder in which red blood cells break down earlier than normal (hemolysis or paroxysmal nocturnal hemoglobinuria)
- White blood cell cancer (Waldenström macroglobulinemia)
Normal Results
Normal RBC ranges are:
- Male: 4.7 to 6.1 million cells per microliter (cells/mcL)
- Female: 4.2 to 5.4 million cells/mcL
The ranges above are common measurements for results of these tests. Normal value ranges may vary slightly among different laboratories. Some labs use different measurements or test different samples. Talk to your health care provider about the meaning of your specific test results.
What Abnormal Results Mean
Higher than normal numbers of RBCs may be due to:
- Bone marrow disease that causes abnormal increase in RBCs (polycythemia vera)
- Cigarette smoking
- Dehydration (for example, from severe diarrhea)
- Failure of the right side of the heart (cor pulmonale)
- Kidney tumor (renal cell carcinoma)
- Low blood oxygen level (hypoxia)
- Problem with heart's structure and function that is present at birth (congenital heart disease)
- Scarring or thickening of the lungs (pulmonary fibrosis)
Your RBC count will increase for several weeks when you are in a higher altitude.
Drugs that can increase the RBC count include:
- Anabolic steroids
- Erythropoietin
- Gentamicin
- Testosterone
Lower-than-normal numbers of RBCs may be due to:
- Anemia
- Bleeding
- Bone marrow cancer called multiple myeloma
- Bone marrow failure (for example, from radiation, toxins, or tumor)
- Deficiency of a hormone called erythropoietin (caused by kidney disease)
- Leukemia
- Malnutrition
- Pregnancy
- RBC destruction (hemolysis) due to transfusion, blood vessel injury, or other cause
- Too little iron, copper, folic acid, vitamin B6, or vitamin B12 in the diet
- Too much water in the body (overhydration)
Drugs that can decrease the RBC count include:
- Chemotherapy drugs
- Chloramphenicol and certain other antibiotics
- Hydantoins
- Methyldopa
- Nonsteroidal anti-inflammatory drugs (NSAIDs)
- Quinidine
Risks
There is little risk involved with having your blood taken. Veins and arteries vary in size from one person to another and from one side of the body to the other. Taking blood from some people may be more difficult than from others.
Other risks associated with having blood drawn are slight, but may include:
- Excessive bleeding
- Fainting or feeling lightheaded
- Multiple punctures to locate veins
- Hematoma (blood buildup under the skin)
- Infection (a slight risk any time the skin is broken)
References
Gallagher PG. Hemolytic anemias: red blood cell membrane and metabolic defects. In: Goldman L, Schafer AI, eds. Goldman-Cecil Medicine. 26th ed. Philadelphia, PA: Elsevier; 2020:chap 152.
Little M. Anaemia. In: Cameron P, Little M, Mitra B, Deasy C, eds. Textbook of Adult Emergency Medicine. 5th ed. Philadelphia, PA: Elsevier; 2020:chap 13.
Pincus MR, Abraham NZ, Bluth M. Interpreting laboratory results. In: McPherson RA, Pincus MR, eds. Henry's Clinical Diagnosis and Management by Laboratory Methods. 24th ed. Philadelphia, PA: Elsevier; 2022:chap 9.
Means RT. Approach to the anemias. In: Goldman L, Schafer AI, eds. Goldman-Cecil Medicine. 26th ed. Philadelphia, PA: Elsevier; 2020:chap 149.
Review Date: 1/9/2022
Reviewed By: David C. Dugdale, III, MD, Professor of Medicine, Division of General Medicine, Department of Medicine, University of Washington School of Medicine. Also reviewed by David Zieve, MD, MHA, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.