Numbness and tingling
Sensory loss; Paresthesias; Tingling and numbness; Loss of sensation; Pins and needles sensation
Numbness and tingling are abnormal sensations that can occur anywhere in your body, but they are often felt in your fingers, hands, feet, arms, or legs.
Causes
There are many possible causes of numbness and tingling, including:
- Sitting or standing in the same position for a long time
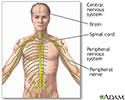
- Injuring a nerve (a neck injury may cause you to feel numbness anywhere along your arm or hand, while a low back injury can cause numbness or tingling down the back of your leg)
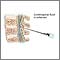
- Pressure on the nerves of the spine, such as from a herniated disk
- Pressure on peripheral nerves from enlarged blood vessels, tumors, scar tissue, or infection
- Shingles or herpes zoster infection
- Other infections such as HIV/AIDS, leprosy, syphilis, or tuberculosis
- Lack of blood supply to an area, such as from hardening of the arteries, frostbite, or vessel inflammation
- Abnormal levels of calcium, potassium, or sodium in your body
- Deficiency of B vitamins such as B1, B6, B12, or folic acid
- Use of certain medicines
- Use of certain illicit street drugs
- Nerve damage due to lead, alcohol, or tobacco, or from chemotherapy drugs
- Radiation therapy
- Animal bites
- Insect, tick, mite, and spider bites
- Seafood toxins
- Congenital conditions that affect the nerves
Numbness and tingling can be caused by other medical conditions, including:
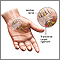
- Carpal tunnel syndrome (pressure on a nerve at the wrist)
- Diabetes
- Migraines
- Multiple sclerosis
- Seizures
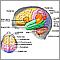
- Stroke
- Transient ischemic attack (TIA), sometimes called a "mini-stroke"
- Underactive thyroid
- Raynaud phenomenon (narrowing of the blood vessels, usually in the hands and feet)
Home Care
Your health care provider should find and treat the cause of your numbness or tingling. Treating the condition may make the symptoms go away or stop them from getting worse. For example, if you have carpal tunnel syndrome or low back pain, your doctor may recommend certain exercises.
If you have diabetes, your provider will discuss ways to control your blood sugar level.
Low levels of vitamins will be treated with vitamin supplements.
Medicines that cause numbness or tingling may need to be switched or changed. DO NOT change or stop taking any of your medicines or take large doses of any vitamins or supplements until you have talked with your provider.
Because numbness can cause a decrease in feeling, you may be more likely to accidentally injure a numb hand or foot. Take care to protect the area from cuts, bumps, bruises, burns, or other injuries. If you have chronic numbness of the feet (such as from diabetes), seeing a podiatrist regularly can help prevent complications.
When to Contact a Medical Professional
Go to a hospital or call your local emergency number (such as 911) if:
- You have weakness or are unable to move, along with numbness or tingling
- Numbness or tingling occur just after a head, neck, or back injury
- You cannot control the movement of an arm or a leg, or you have lost bladder or bowel control
- You are confused or have lost consciousness, even briefly
- You have slurred speech, a change in vision, difficulty walking, or weakness
Call your provider if:
- Numbness or tingling has no obvious cause (like a hand or foot "falling asleep")
- You have pain in your neck, forearm, or fingers
- You are urinating more often
- Numbness or tingling is in your legs and gets worse when you walk
- You have a rash
- You have dizziness, muscle spasm, or other unusual symptoms
What to Expect at Your Office Visit
Your provider will take a medical history and perform a physical examination, carefully checking your nervous system.
You will be asked about your symptoms. Questions may include when the problem began, its location, or if there's anything that improves or worsens the symptoms.
Your provider may also ask questions to determine your risk for stroke, thyroid disease, or diabetes, as well as questions about your work habits and medicines.
Blood tests that may be ordered include:
- Complete blood count (CBC)
- Electrolyte level (measurement of body chemicals and minerals) and liver function tests
- Thyroid function tests
- Measurement of vitamin levels, particularly vitamin B12
- Heavy metal or toxicology screening
- Sedimentation rate
- C-reactive protein
Imaging tests may include:
- Angiogram (a test that uses x-rays and a special dye to see inside the blood vessels)
- CT angiogram
- CT scan of the head
- CT scan of the spine
- MRI of the head
- MRI of the spine
- Ultrasound of neck vessels to determine your risk for TIA or stroke
- Vascular ultrasound
- X-ray of the affected area
Other tests that may be done include:
- Electromyography and nerve conduction studies to measure how your muscles respond to nerve stimulation
- Lumbar puncture (spinal tap) to rule out central nervous system disorders
- Cold stimulation test may be done to check for Raynaud phenomenon
- Genetic testing for nerve problems that run in families.
References
McGee S. Examination of the sensory system. In: McGee S, ed. Evidence-Based Physical Diagnosis. 5th ed. Philadelphia, PA: Elsevier; 2022:chap 62.
Snow DC, Bunney BE. Peripheral nerve disorders. In: Walls RM, Hockberger RS, Gausche-Hill M, eds. Rosen's Emergency Medicine: Concepts and Clinical Practice. 9th ed. Philadelphia, PA: Elsevier; 2018:chap 97.
Swartz MH. The nervous system. In: Swartz MH, ed. Textbook of Physical Diagnosis: History and Examination. 8th ed. Philadelphia, PA: Elsevier; 2021:chap 21.
Review Date: 5/4/2021
Reviewed By: Joseph V. Campellone, MD, Department of Neurology, Cooper Medical School at Rowan University, Camden, NJ. Review provided by VeriMed Healthcare Network. Also reviewed by David Zieve, MD, MHA, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.