Anorectal abscess
Anal abscess; Rectal abscess; Perirectal abscess; Perianal abscess; Gland abscess; Abscess - anorectal
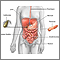
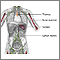
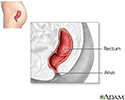
An anorectal abscess is a collection of pus in the area of the anus and rectum.
Causes
Common causes of anorectal abscess include:
- Blocked glands in the anal area
- Infection of an anal fissure
- Sexually transmitted infection (STD)
- Trauma
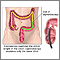
Deep rectal abscesses may be caused by intestinal disorders such as Crohn disease or diverticulitis.
The following factors increase the risk for an anorectal abscess:
- Anal sex
- Chemotherapy medicines used to treat cancer
- Diabetes
- Inflammatory bowel disease (Crohn disease and ulcerative colitis)
- Use of corticosteroid medicines
- Weakened immune system (such as from HIV/AIDS)
The condition affects men more than women. The condition may occur in infants and toddlers who are still in diapers and who have a history of anal fissures.
Symptoms
Common symptoms are swelling around the anus and a constant, throbbing pain with swelling. Pain may be severe with bowel movements, coughing and sitting.
Other symptoms may include:
- Constipation
- Discharge of pus from the rectum
- Fatigue, fever, night sweats, and chills
- Redness, painful and hardened tissue in the area of the anus
- Tenderness
In infants, the abscess often appears as a swollen, red, tender lump at the edge of the anus. The infant may be fussy and irritable from discomfort. There are usually no other symptoms.
Exams and Tests
A rectal examination may confirm an anorectal abscess. A proctosigmoidoscopy may be done to rule out other diseases.
In some cases, a CT scan, MRI, or ultrasound is needed to help locate the collection of pus.
Treatment
The problem rarely goes away on its own. Antibiotics alone usually cannot treat an abscess.
Treatment involves surgery to open and drain the abscess.
- Surgery is usually done with local numbing medicine, along with medicine to make you sleepy. Sometimes, spinal or general anesthesia is used.
- Surgery is most often an outpatient procedure, which means that you go home on the same day. The surgeon cuts open the abscess and drains the pus. Sometimes a drain is put in to keep the incision open and draining, and sometimes the abscess cavity is packed with gauze.
- If the pus collection is deep, you may need to stay in the hospital longer for pain control and nursing care of the abscess drainage site.
- After surgery, you may need warm sitz baths (sitting in a tub of warm water). This helps relieve pain and reduce swelling.
Drained abscesses are usually left open and no stitches are needed.
The surgeon may prescribe painkillers and antibiotics.
Avoiding constipation will help decrease pain. You may need stool softeners. Drinking fluids and eating foods with lots of fiber can also help.
Outlook (Prognosis)
With prompt treatment, people with this condition usually do well. Infants and toddlers usually recover quickly.
Complications can occur when treatment is delayed.
Possible Complications
Complications of anorectal abscess may include:
- Anal fistula (abnormal connection between the anus and another structure)
- Infection that spreads to the blood (sepsis)
- Continuing pain
- Problem keeps coming back (recurrence)
When to Contact a Medical Professional
Call your health care provider if you:
- Notice rectal discharge, pain, or other symptoms of anorectal abscess
- Have fever, chills, or other new symptoms after being treated for this condition
- Are a diabetic and your blood glucose becomes difficult to control
Prevention
Prevention or prompt treatment of STDs may prevent an anorectal abscess from forming. Use condoms during intercourse, including anal sex, to prevent such infections.
In infants and toddlers, frequent diaper changes and proper cleaning during diaper changes can help prevent both anal fissures and abscesses.
References
Coates WC. Anorectal procedures. In: Roberts JR, Custalow CB, Thomsen TW, eds. Roberts and Hedges' Clinical Procedures in Emergency Medicine and Acute Care. 7th ed. Philadelphia, PA: Elsevier; 2019:chap 45.
Hyman N, Omanskiy K. Anus. In: Townsend CM Jr, Beauchamp RD, Evers BM, Mattox KL, eds. Sabiston Textbook of Surgery. 21st ed. Philadelphia, PA: Elsevier; 2022:chap 53.
Review Date: 4/20/2022
Reviewed By: Debra G. Wechter, MD, FACS, General Surgery Practice Specializing in Breast Cancer, Virginia Mason Medical Center, Seattle, WA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.