Axillary nerve dysfunction
Neuropathy - axillary nerve
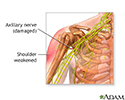
Axillary nerve dysfunction is nerve damage that can lead to a loss of movement or sensation in the shoulder.
Causes
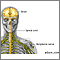
Axillary nerve dysfunction is a form of peripheral neuropathy. It occurs when there is damage to the axillary nerve. This is the nerve that helps control the deltoid muscles of the shoulder and the skin around it. A problem with just one nerve, such as the axillary nerve, is called mononeuropathy.
The usual causes are:
- Direct injury
- Long-term pressure on the nerve
- Pressure on the nerve from nearby body structures
- Shoulder injury
Entrapment creates pressure on the nerve where it passes through a narrow structure.
The damage can destroy the myelin sheath that covers the nerve or part of the nerve cell (the axon). Damage of either type reduces or prevents the movement of signals through the nerve.
Conditions that can lead to axillary nerve dysfunction include:
- Body-wide (systemic) disorders that cause nerve inflammation
- Deep infection
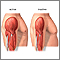
- Fracture of the upper arm bone (humerus)
- Pressure from casts or splints
- Improper use of crutches
- Shoulder dislocation
In some cases, no cause can be found.
Symptoms
Symptoms may include any of the following:
- Numbness over part of the outer shoulder
- Shoulder weakness, especially when lifting the arm up and away from the body
Exams and Tests
Your health care provider will examine your neck, arm, and shoulder. Weakness of the shoulder can cause difficulty moving your arm.
The deltoid muscle of the shoulder may show signs of muscle atrophy (loss of muscle tissue and thinning).
Tests that may be used to check axillary nerve dysfunction include:
- EMG and nerve conduction tests will likely be normal right after the injury and should be done several weeks after the injury or symptoms start
- MRI or x-rays of the shoulder
Treatment
Depending on the cause of the nerve disorder, some people do not need treatment. The problem may get better on its own. The rate of recovery is different for everyone. It can take many months to recover.
Anti-inflammatory medicines may be given if you have any of the following:
- Sudden symptoms
- Small changes in sensation or movement
- No history of injury to the area
- No signs of nerve damage
These medicines reduce swelling and pressure on the nerve. They may be injected directly into the area or taken by mouth.
Other medicines include:
- Over-the-counter pain medicines may be helpful for mild pain (neuralgia).
- Medicines to help reduce stabbing pain.
- Opiate pain relievers may be needed to control severe pain.
If your symptoms continue or get worse, you may need surgery. If a trapped nerve is causing your symptoms, surgery to release the nerve may help you feel better.
Physical therapy can help maintain muscle strength. Job changes, muscle retraining, or other forms of therapy may be recommended.
Outlook (Prognosis)
It may be possible to make a full recovery if the cause of the axillary nerve dysfunction can be identified and successfully treated.
Possible Complications
Complications may include:
- Deformity of the arm, shoulder contracture, or frozen shoulder
- Partial loss of sensation in the arm (uncommon)
- Partial shoulder paralysis
- Repeated injury to the arm
When to Contact a Medical Professional
Call for an appointment with your provider if you have symptoms of axillary nerve dysfunction. Early diagnosis and treatment increase the chance of controlling symptoms.
Prevention
Preventive measures vary, depending on the cause. Avoid putting pressure on the underarm area for long periods. Make sure casts, splints, and other appliances fit properly. When you use crutches, learn how to avoid putting pressure on the underarm.
References
Hess DE, Taylor KF, Chhabra AB. Nerve entrapment. In: Miller MD, Thompson SR, eds. DeLee, Drez, & Miller's Orthopaedic Sports Medicine. 5th ed. Philadelphia, PA: Elsevier; 2020:chap 54.
Pierrie SN, Loeffler BJ. Common nerve injuries about the shoulder. In: Skirven TM, Osterman AL, Fedroczyk JM, Amadio PC, Feldscher SB, Shin EK, eds. Rehabilitation of the Hand and Upper Extremity. 7th ed. Philadelphia, PA: Elsevier; 2021:chap 47.
Review Date: 1/28/2021
Reviewed By: Evelyn O. Berman, MD, Assistant Professor of Neurology and Pediatrics at University of Rochester, Rochester, NY. Review provided by VeriMed Healthcare Network. Also reviewed by David Zieve, MD, MHA, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.