Analgesic nephropathy
Phenacetin nephritis; Nephropathy - analgesic; Nephropathy - NSAID
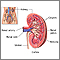
Analgesic nephropathy involves damage to one or both kidneys caused by overexposure to mixtures of medicines, especially over-the-counter pain medicines (analgesics).
Causes
Analgesic nephropathy involves damage within the internal structures of the kidney. It is caused by long-term use of analgesics (pain medicines), especially over-the-counter (OTC) medicines that contain phenacetin or acetaminophen, and nonsteroidal anti-inflammatory drugs (NSAIDs), such as aspirin or ibuprofen.
This condition frequently occurs as a result of self-medicating, often for some type of chronic pain.
Risk factors include:
- Use of OTC analgesics containing more than one active ingredient
- Taking 6 or more pills a day for 3 years
- Chronic headaches, painful menstrual periods, backache, or musculoskeletal pain
- Emotional or behavioral changes
- History of dependent behaviors including smoking, alcohol use, and excessive use of tranquilizers
Symptoms
There may be no symptoms in the beginning. Over time, as the kidneys are injured by the medicine, symptoms of kidney disease will develop, including:
- Fatigue, weakness
- Increased urinary frequency or urgency
- Blood in the urine
- Flank pain or back pain
- Decreased urine output
- Decreased alertness, including drowsiness, confusion, and lethargy
- Decreased sensation, numbness (especially in the legs)
- Nausea, vomiting
- Easy bruising or bleeding
- Swelling (edema) throughout the body
Exams and Tests
The health care provider will examine you and ask about your symptoms. During the exam, your provider may find:
- Your blood pressure is high.
- When listening with a stethoscope, your heart and lungs have abnormal sounds.
- You have swelling, especially in the lower legs.
- Your skin shows premature aging.
Tests that may be done include:
- Complete blood count
- CT scan of kidney
- Intravenous pyelogram (IVP)
- Toxicology screen
- Urinalysis
- Kidney ultrasound
Treatment
The primary goals of treatment are to prevent further damage of the kidneys and to treat kidney failure. Your provider may tell you to stop taking all suspect painkillers, particularly OTC medicines.
To treat kidney failure, your provider may suggest diet changes and fluid restriction. Eventually, dialysis or a kidney transplant may be needed.
Counseling may help you develop alternative methods of controlling chronic pain.
Outlook (Prognosis)
The damage to the kidney may be acute and temporary, or chronic and long term.
Possible Complications
Complications that may result from analgesic nephropathy include:
- Acute kidney failure
- Chronic kidney failure
- Kidney disorder in which the spaces between the kidney tubules become inflamed (interstitial nephritis)
- Tissue death in areas where the openings of the collecting ducts enter the kidney and where urine flows into the ureters (renal papillary necrosis)
- Urinary tract infections that are ongoing or keep coming back
- High blood pressure
- Cancer of the kidney or ureter
When to Contact a Medical Professional
Contact your provider if you have any of the following:
- Symptoms of analgesic nephropathy, especially if you have been using painkillers for a long time
- Blood or solid material in your urine
- Amount of your urine has decreased
Prevention
Follow your provider's instructions when using medicines, including OTCs. Do not take more than the recommended dose without asking your provider.
References
Aronson JK. Paracetamol (acetaminophen) and combinations. In: Aronson JK, eds. Meyler's Side Effects of Drugs. 16th ed. Waltham, MA: Elsevier; 2016:474-493.
Parazella MA, Rosner MH. Tubulointerstitial diseases. In: Yu ASL, Chertow GM, Luyckx VA, Marsden PA, Skorecki K, Taal MW, eds. Brenner and Rector's The Kidney. 11th ed. Philadelphia, PA: Elsevier; 2020:chap 35.
Segal MS, Yu X. Herbal and over-the-counter medicines and the kidney. In: Feehally J, Floege J, Tonelli M, Johnson RJ, eds. Comprehensive Clinical Nephrology. 6th ed. Philadelphia, PA: Elsevier; 2019:chap 76.
Review Date: 7/27/2021
Reviewed By: Walead Latif, MD, Nephrologist and Clinical Associate Professor, Rutgers Medical School, Newark, NJ. Review provided by VeriMed Healthcare Network. Also reviewed by David Zieve, MD, MHA, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.