Severe COVID-19 - discharge
Severe coronavirus 2019 - discharge; Severe SARS-CoV-2 - discharge
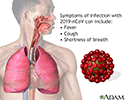
You have been in the hospital with COVID-19, which causes an infection in your lungs and may cause problems with other organs, including the kidneys, heart, and liver. Most often it causes a respiratory illness with fever, coughing, and shortness of breath. Now that you are going home, follow your health care provider's instructions on taking care of yourself at home. Use the information below as a reminder.
When You're in the Hospital
In the hospital, your health care providers gave treatment to help you breathe better. They may give you oxygen and IV fluids (given through a vein) and nutrients. You may be intubated and on a ventilator. If your kidneys are injured, you may have dialysis. You also may receive medicines to help you recover.
Once you can breathe on your own and your symptoms improve, you may spend time in a rehabilitation facility to build up your strength before going home. Or you may go directly home.
What to Expect at Home
Once at home, your provider will continue to work with you to help your recovery.
You will likely still have symptoms of COVID-19 even after you leave the hospital.
- You may need to use oxygen at home as you recover.
- You may still have a cough that slowly gets better.
- You may have kidneys that have not recovered fully.
- You may get tired easily and sleep a lot.
- You may not feel like eating. You may not be able to taste and smell food.
- You may feel mentally foggy or have memory loss.
- You may feel anxious or depressed.
- You may have other bothersome symptoms, such as headache, diarrhea, joint or muscle pain, heart palpitations, and trouble sleeping.
Recovery may take weeks or even months. Some people will have ongoing symptoms.
Be sure to follow your provider's instructions for self-care at home. They may include some of the following recommendations.
MEDICINES
Your provider may prescribe medicines to help in your recovery, such as antibiotics or blood thinners. Be sure to take your medicine as prescribed. Do not miss any doses.
DO NOT take cough or cold medicines unless your provider says it is OK. Coughing helps your body get rid of mucus from your lungs.
Your provider will tell you if it is OK to use acetaminophen (Tylenol) or ibuprofen (Advil or Motrin) for pain. If these medicines are OK to use, your provider will tell you how much to take and how often to take them.
OXYGEN THERAPY
Your provider may prescribe oxygen for you to use at home. Oxygen helps you breathe better.
- Never change how much oxygen is flowing without asking your provider or respiratory therapist.
- Always have a back-up supply of oxygen at home or with you when you go out.
- Keep the phone number of your oxygen supplier with you at all times.
- Learn how to use oxygen safely at home.
- Never smoke near an oxygen tank.
If you smoke, now is the time to quit. Do not allow smoking in your home.
BREATHING EXERCISES
Doing breathing exercises every day may be important to help strengthen the muscles you use to breathe and help open up your airways. Your provider may give you instructions on how to do breathing exercises. This may include:
Incentive spirometry - You may be sent home with a spirometer to use several times a day. This is a hand-held clear plastic device with a breathing tube and a movable gauge. You take long, sustained breaths to keep the gauge at the level your provider specified.
Rhythmic inhalation and coughing - Breathe deeply several times and then cough. This may help bring up mucus from your lungs.
Chest tapping - While lying down, tap your chest gently a few times a day. This may help bring up mucus from the lungs.
You may find that these exercises are not easy to do, but doing them every day may help you recover your lung function more quickly.
NUTRITION
Lingering COVID-19 symptoms including loss of taste and smell, nausea, or tiredness can make it hard to want to eat. Eating a healthy diet is important for your recovery. These suggestions may help:
- Try to eat healthy foods you enjoy most of the time. Eat anytime you feel like eating, not just at mealtime.
- Include a variety of fruits, vegetables, whole grains, dairy, and protein foods. Include a protein food with every meal (tofu, beans, legumes, cheese, fish, poultry, or lean meats)
- Try adding herbs, spices, onion, garlic, ginger, hot sauce or spice, mustard, vinegar, pickles, and other strong flavors to help increase enjoyment.
- Try foods with different textures and temperatures to see what is more appealing.
- Eat smaller meals more often throughout the day.
- If you need to gain weight, your provider may recommend adding full-fat yogurt, cheese, cream, butter, powdered milk, oils, nuts and nut butters, honey, syrups, jams, and other high-calorie foods to meals to add extra calories.
- For snacks, try milkshakes or smoothies, fruit and fruit juices, and other nutritious foods.
- Your provider also may recommend a nutrition or vitamin supplement to help ensure you get all the nutrients you need.
Being short of breath can also make it harder to eat. To make it easier:
- Eat smaller portions more often throughout the day.
- Eat softer foods that you can easily chew and swallow.
- Don't rush your meals. Take small bites and breathe as you need to in between bites.
Drink plenty of liquids, as long as your provider says it is OK. Just don't fill up on liquids before or during your meals.
- Drink water, juice, or weak tea.
- Drink at least 6 to 10 cups (1.5 to 2.5 liters) a day.
- Do not drink alcohol.
EXERCISE
Even though you don't have a lot of energy, it's important to move your body every day. This will help you regain your strength.
- Follow your provider's recommendation for activity.
- You may find it easier to breathe lying on your stomach with a pillow under your chest.
- Try to change and move positions throughout the day, and sit upright as much as you are able.
- Try walking around your home for short periods every day. Try walking 5 minutes, 5 times a day. Slowly build up every week.
- If you are given a pulse oximeter, use it to check your heart rate and oxygen level. Stop and rest if your oxygen goes too low. Report to your provider if readings continue to be low.
MENTAL HEALTH
It is common for people who have been hospitalized with COVID-19 to experience a range of emotions, including anxiety, depression, sadness, isolation, and anger. Some people experience post-traumatic stress disorder (PSTD) as a result.
Many of the things you do to help with your recovery, such as a healthy diet, regular activity, and enough sleep, will also help you keep a more positive outlook.
You can help reduce stress by practicing relaxation techniques such as:
- Meditation
- Progressive muscle relaxation
- Gentle yoga
Avoid social isolation by reaching out to people you trust by phone calls, social media, or video calls. Talk about your experience and how you are feeling.
Call your health care provider right away if feelings of sadness, anxiety, or depression:
- Affect your ability to help yourself recover
- Make it hard to sleep
- Feel overwhelming
- Make you feel like hurting yourself
When to Call the Doctor
Call 911 or the local emergency number if symptoms re-appear, or you notice worsening of symptoms such as:
- Difficulty breathing
- Pain or pressure in the chest
- Weakness or numbness in a limb or one side of the face
- Confusion
- Seizures
- Slurred speech
- Bluish, gray, or pale discoloration of lips or face
- Swelling of the legs or arms
- Any other symptoms that are severe or concern you
References
Centers for Disease Control and Prevention website. COVID-19: Treatments and medications. www.cdc.gov/coronavirus/2019-ncov/your-health/treatments-for-severe-illness.html. Updated January 26, 2023. Accessed January 31, 2023.
National Institutes of Health. COVID-19 Treatment Guidelines: What's new in the guidelines. www.covid19treatmentguidelines.nih.gov/about-the-guidelines/whats-new/. Updated January 30, 2023. Accessed January 31, 2023.
National Institutes of Health website. COVID-19 treatment guidelines. Therapeutic management of hospitalized adults with COVID-19. www.covid19treatmentguidelines.nih.gov/management/clinical-management/hospitalized-adults--therapeutic-management/. Updated August 8, 2022. Accessed January 31, 2023.
Prescott HC, Girard TD. Recovery From Severe COVID-19: Leveraging the Lessons of Survival From Sepsis. JAMA. 2020;324(8):739-740. PMID: 32777028 pubmed.ncbi.nlm.nih.gov/32777028/.
Spruit MA, Holland AE, Singh SJ, Tonia T, Wilson KC, Troosters T. COVID-19: Interim Guidance on Rehabilitation in the Hospital and Post-Hospital Phase from a European Respiratory Society and American Thoracic Society-coordinated International Task Force [published online ahead of print, 2020 Dec 3]. Eur Respir J. 2020 Dec; 56(6): 2002197. PMID: 32817258 pubmed.ncbi.nlm.nih.gov/32817258/.
Review Date: 2/22/2023
Reviewed By: Frank D. Brodkey, MD, FCCM, Associate Professor, Section of Pulmonary and Critical Care Medicine, University of Wisconsin School of Medicine and Public Health, Madison, WI. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.