Diverticulosis
Diverticula - diverticulosis; Diverticular disease - diverticulosis; G.I. bleed - diverticulosis; Gastrointestinal hemorrhage - diverticulosis; Gastrointestinal bleed - diverticulosis; Jejunal diverticulosis
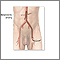
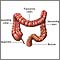
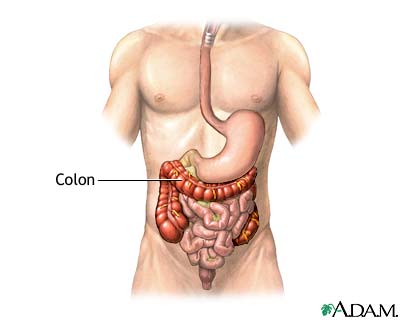
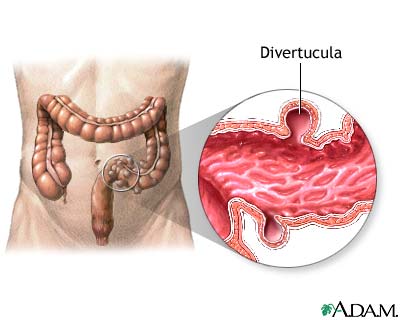
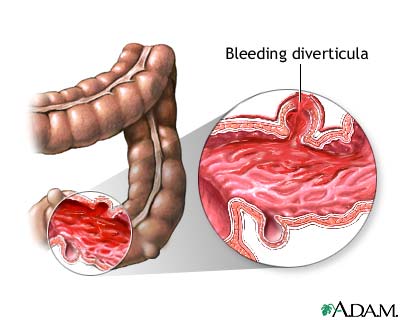
Diverticulosis occurs when small, bulging sacs or pouches form on the inner wall of the intestine. These sacs are called diverticula. Most often, these pouches form in the large intestine (colon). They may also occur in the jejunum in the small intestine, although this is less common.
Causes
Diverticulosis is less common in people age 40 and younger. It's more common in older adults. About half of Americans over age 60 have this condition. Most people will have it by age 80.
No one knows exactly what causes these pouches to form.
For many years, it was thought that eating a low-fiber diet may play a role. Not eating enough fiber can cause constipation (hard stools). Straining to pass stools (feces) increases the pressure in the colon or intestines. This may cause the pouches to form at weak spots in the colon wall. However, whether a low-fiber diet leads to this problem is not well proven.
Other possible risk factors that are also not well proven are lack of exercise and obesity.
Eating nuts, popcorn, or corn does not appear to lead to inflammation of these pouches (diverticulitis).
Symptoms
Most people with diverticulosis have no symptoms.
When symptoms occur, they may include:
- Pain and cramps in your stomach especially in the left lower abdomen
- Constipation (sometimes diarrhea)
- Bloating or gas
- Not feeling hungry and not eating
You may notice small amounts of blood in your stools or on toilet paper. Rarely, more severe bleeding may occur.
Exams and Tests
Diverticulosis is often found during an exam for another health problem. For example, it is often discovered during a colonoscopy.
If you do have symptoms, you may have one or more of the following tests:
- Blood tests to see if you have an infection or have lost too much blood
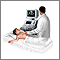
- CT scan or ultrasound of the abdomen if you have bleeding, loose stools, or pain
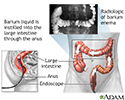
A colonoscopy is needed to make the diagnosis:
- A colonoscopy is an exam that views the inside of the colon and rectum. This test should not be done when you are having symptoms of acute diverticulitis.
- A small camera attached to a tube can reach the length of the colon.
- Angiography is an imaging test that uses x-rays and a special dye to see inside the blood vessels.
- This test may be used if the area of bleeding is not seen during a colonoscopy.
Treatment
Because most people have no symptoms, most of the time, no treatment is needed.
Your health care provider may recommend getting more fiber in your diet. A high-fiber diet has many health benefits. Most people don't get enough fiber. To help prevent constipation, you should:
- Eat plenty of whole grains, beans, fruits, and vegetables. Limit processed foods.
- Drink plenty of fluids.
- Get regular exercise.
- Talk with your provider about taking a fiber supplement.
You should avoid NSAIDs such as aspirin, ibuprofen (Motrin), and naproxen (Aleve). These medicines can make bleeding more likely.
For bleeding that does not stop or recurs:
- Colonoscopy may be used to inject medicines or burn a certain area in the intestine to stop the bleeding.
- Angiography may be used to infuse medicines or block off a blood vessel.
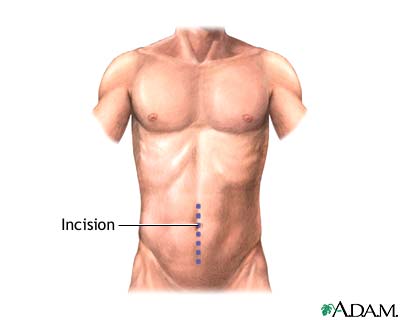
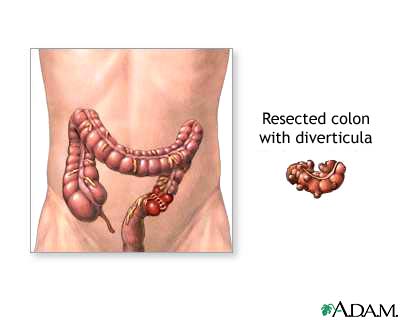
If bleeding does not stop or recurs many times, removal of a section of the colon may be needed.
Outlook (Prognosis)
Most people who have diverticulosis have no symptoms. Once these pouches have formed, you will have them for life.
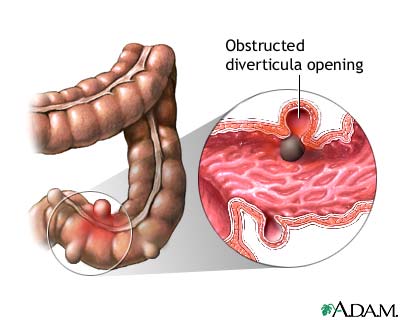
Up to 25% of people with the condition will develop diverticulitis. This occurs when small pieces of stool become trapped in the pouches, causing infection or swelling.
Possible Complications
More serious problems that may develop include:
- Abnormal connections that form between parts of the colon or between the colon and another part of the body (fistula)
- Hole or tear in the colon (perforation)
- Narrowed area in the colon (stricture)
- Pockets filled with pus or infection (abscess)
When to Contact a Medical Professional
Call your provider if symptoms of diverticulitis occur.
References
Bhuket TP, Stollman NH. Diverticular disease of the colon. In: Feldman M, Friedman LS, Brandt LJ, eds. Sleisenger and Fordtran's Gastrointestinal and Liver Disease. 11th ed. Philadelphia, PA: Elsevier; 2021:chap 121.
Goldblum JR. Large bowel. In: Goldblum JR, Lamps LW, McKenney JK, Myers JL, eds. Rosai and Ackerman's Surgical Pathology. 11th ed. Philadelphia, PA: Elsevier; 2018:chap 17.
Fransman RB, Harmon JW. The management of diverticulosis of the small bowel. In: Cameron AM, Cameron JL, eds. Current Surgical Therapy. 13th ed. Philadelphia, PA: Elsevier; 2020:143-145.
Winter D, Ryan E. Diverticular disease. In: Clark S, ed. Colorectal Surgery: A Companion to Specialist Surgical Practice. 6th ed. Philadelphia, PA: Elsevier; 2019:chap 10.
Review Date: 10/27/2021
Reviewed By: Michael M. Phillips, MD, Emeritus Professor of Medicine, The George Washington University School of Medicine, Washington, DC. Also reviewed by David Zieve, MD, MHA, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.