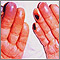
Fingers that change color
Blanching of the fingers; Fingers - pale; Toes that change color; Toes - pale
Fingers or toes may change color when they are exposed to cold temperatures or stress, or when there is a problem with their blood supply.
Causes
These conditions can cause fingers or toes to change color:
- Buerger disease
- Chilblains (painful inflammation of small blood vessels)
- Cryoglobulinemia
- Frostbite
- Necrotizing vasculitis
- Peripheral artery disease
- Raynaud phenomenon (sudden change in the finger color ranges from pale to red to blue)
- Scleroderma
- Systemic lupus erythematosus
Home Care
Things you can do to help prevent this problem include:
- Avoid smoking.
- Avoid exposure to cold in any form.
- Wear mittens or gloves outdoors and when handling ice or frozen food.
- Avoid getting chilled, which may happen following any active recreational sport or other physical activity.
- Wear comfortable, roomy shoes and wool socks.
- When outside, always wear shoes.
When to Contact a Medical Professional
Call your health care provider if:
- Your fingers change color and the cause is not known.
- Your fingers or toes turn black or the skin breaks.
What to Expect at Your Office Visit
Your provider will perform a physical exam, which will include close examination of your hands, arms, and fingers.
Your provider will ask questions about your medical history and symptoms, including:
- Did the fingers or toes suddenly change color?
- Has the color change occurred before?
- Does the cold or changes in your emotions cause your fingers or toes to turn white or blue?
- Did the skin color changes occur after you had anesthesia?
- Do you smoke?
- Do you have other symptoms such as finger pain? Arm or leg pain? A change in the texture of your skin? Loss of hair on your arms or hands?
Tests that may be done include:
- Antinuclear antibody blood test
- Blood differential
- Complete blood count (CBC)
- Comprehensive metabolic panel
- Duplex Doppler ultrasound of the arteries to the extremities
- Serum cryoglobulins
- Serum protein electrophoresis
- Urinalysis
- X-ray of your hands and feet
Treatment depends on the underlying cause.
References
Jaff MR, Bartholomew JR. Other peripheral arterial diseases. In: Goldman L, Schafer AI, eds. Goldman-Cecil Medicine. 26th ed. Philadelphia, PA: Elsevier; 2020:chap 72.
Robert A, Melville I, Baines CP, Belch JJF. Raynaud phenomenon. In: Hochberg MC, Gravallese EM, Silman AJ, Smolen JS, Weinblatt ME, Weisman MH, eds. Rheumatology. 7th ed. Philadelphia, PA: Elsevier; 2019:chap 154.
Raynaud's phenomenon - illustration
Raynaud's phenomenon
illustration
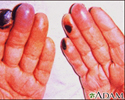
Cryoglobulinemia of the fingers - illustration
Cryoglobulinemia of the fingers
illustration
Review Date: 5/3/2021
Reviewed By: Linda J. Vorvick, MD, Clinical Associate Professor, Department of Family Medicine, UW Medicine, School of Medicine, University of Washington, Seattle, WA. Also reviewed by David Zieve, MD, MHA, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.