Miscarriage
Abortion - spontaneous; Spontaneous abortion; Abortion - missed; Abortion - incomplete; Abortion - complete; Abortion - inevitable; Abortion - infected; Missed abortion; Incomplete abortion; Complete abortion; Inevitable abortion; Infected abortion
A miscarriage is the spontaneous loss of a fetus before the 20th week of pregnancy. Pregnancy losses after the 20th week are called stillbirths. Miscarriage is a naturally occurring event, unlike medical or surgical abortions.
A miscarriage may also be called a "spontaneous abortion." Other terms for the early loss of pregnancy include:
- Complete abortion: All of the products (tissue) of conception leave the body.
- Incomplete abortion: Only some of the products of conception leave the body.
- Inevitable abortion: Symptoms cannot be stopped and a miscarriage will happen.
- Infected (septic) abortion: The lining of the womb (uterus) and any remaining products of conception become infected.
- Missed abortion: The pregnancy has failed and the products of conception do not leave the body.
Your health care provider may also use the term "threatened miscarriage." The symptoms of this condition are abdominal cramps with or without vaginal bleeding. They are a sign that a miscarriage may occur.
Causes
Most miscarriages are caused by chromosome problems that make it impossible for the baby to develop. In rare cases, these problems are related to the mother's or father's genes.
Other possible causes of miscarriage may include:
- Drug and alcohol abuse
- Clotting disorders
- Exposure to environmental toxins
- Hormone problems
- Infection
- Overweight
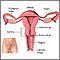
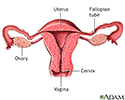
- Physical problems with the mother's reproductive organs
- Problem with the body's immune response
- Serious body-wide (systemic) diseases in the mother (such as uncontrolled diabetes)
- Smoking
Around half of all fertilized eggs die and are lost (aborted) spontaneously, usually before the woman knows she is pregnant. Among women who know they are pregnant, about 10% to 25% will have a miscarriage. Most miscarriages occur during the first 7 weeks of pregnancy. The rate of miscarriage drops after the baby's heartbeat is detected.
The risk for miscarriage is higher:
- In women who are older -- The risk increases after 30 years of age and becomes even greater between 35 and 40 years, and is highest after age 40.
- In women who have already had one or more miscarriages.
Symptoms
Possible symptoms of miscarriage may include:
- Low back pain or abdominal pain that is dull, sharp, or cramping
- Tissue or clot-like material that passes from the vagina
- Vaginal bleeding, with or without abdominal cramps
Some women may not have any symptoms at the beginning.
Exams and Tests
During a pelvic exam, your provider may see that your cervix has opened (dilated).
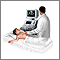
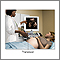
Abdominal or vaginal ultrasound may be done to check the baby's development and heartbeat, and the amount of your bleeding.
The following blood tests may be performed:
- Blood type (if you have an Rh-negative blood type, you would require a treatment with Rh-immune globulin).
- Complete blood count (CBC) to determine how much blood has been lost.
- HCG (qualitative) to confirm pregnancy.
- HCG (quantitative) done every several days or weeks.
- White blood count (WBC) and differential to check for infection.
Treatment
When a miscarriage occurs, the tissue passed from the vagina should be examined. This is done to determine if it was a normal placenta or a rare condition known as a hydatidiform mole. It is also important to find out whether any pregnancy tissue remains in the uterus. In rare cases an ectopic pregnancy can look like a miscarriage. If you have passed tissue, ask your provider if the tissue should be sent for genetic testing. This can be helpful to determine if a treatable cause of miscarriage is present.
If the pregnancy tissue does not naturally leave the body, you may be closely watched for up to 2 weeks. Surgery (suction curettage, D and C) or medicine may be needed to remove the remaining contents from your womb.
After treatment, women usually resume their normal menstrual cycle within 4 to 6 weeks. Any further vaginal bleeding should be carefully monitored. It is often possible to become pregnant immediately. It is suggested that you wait one normal menstrual cycle before trying to become pregnant again.
Possible Complications
In rare cases, complications of miscarriage are seen.
An infected abortion may occur if any tissue from the placenta or fetus remains in the uterus after the miscarriage. Symptoms of an infection include fever, vaginal bleeding that does not stop, cramping, and a foul-smelling vaginal discharge. Infections can be serious and need immediate medical attention.
Women who lose a baby after 20 weeks of pregnancy receive different medical care. This is called premature delivery or fetal demise. This needs immediate medical attention.
After a miscarriage, women and their partners may feel sad. This is normal. If your feelings of sadness do not go away or get worse, seek advice from family and friends as well as your provider. However, for most couples, a history of a miscarriage doesn't reduce the chances of having a healthy baby in the future.
When to Contact a Medical Professional
Contact your provider if you:
- Have vaginal bleeding with or without cramping during pregnancy.
- Are pregnant and notice tissue or clot-like material that passes through your vagina. Collect the material and bring it to your provider for examination.
Prevention
Early, complete prenatal care is the best prevention for complications of pregnancy, such as miscarriage.
Miscarriages that are caused by systemic diseases can be prevented by detecting and treating the disease before pregnancy occurs.
Miscarriages are also less likely if you avoid things that are harmful to your pregnancy. These include x-rays, recreational drugs, alcohol, high caffeine intake, and infectious diseases.
When a mother's body has difficulty keeping a pregnancy, signs such as slight vaginal bleeding may occur. This means there is a risk for miscarriage. But it does not mean one will definitely occur. A pregnant woman who develops any signs or symptoms of threatened miscarriage should contact her prenatal provider instantly.
Taking a prenatal vitamin or folic acid supplement before you become pregnant can greatly lower the chances of miscarriage and certain birth defects.
References
Henn MC, Lall MD. Complications of pregnancy. In: Walls RM, ed. Rosen's Emergency Medicine: Concepts and Clinical Practice. 10th ed. Philadelphia, PA: Elsevier; 2023:chap 173.
Jauniaux ERM, Simpson JL. Pregnancy loss. In: Landon MB, Galan HL, Jauniaux ERM, et al, eds. Gabbe's Obstetrics: Normal and Problem Pregnancies. 8th ed. Philadelphia, PA: Elsevier; 2021:chap 33.
Reddy UM, Silver RM. Stillbirth. In: Lockwood CJ, Copel JA, Dugoff L, et al, eds. Creasy and Resnik's Maternal-Fetal Medicine: Principles and Practice. 9th ed. Philadelphia, PA: Elsevier; 2023:chap 42.
Turocy J, Williams Z. Early and recurrent pregnancy loss; etiology, diagnosis, treatment. In: Gershenson DM, Lentz GM, Valea FA, Lobo RA, eds. Comprehensive Gynecology. 8th ed. Philadelphia, PA: Elsevier; 2022:chap 16.
Review Date: 11/10/2022
Reviewed By: John D. Jacobson, MD, Department of Obstetrics and Gynecology, Loma Linda University School of Medicine, Loma Linda, CA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.