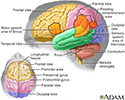
Neurocognitive disorder
Organic mental disorder (OMS); Organic brain syndrome
Neurocognitive disorder is a general term that describes decreased mental function due to a medical disease other than a psychiatric illness.
Neurocognitive disorders are grouped into three subcategories:
- Delirium.
- Mild neurocognitive disorder - some decreased mental function, but able to stay independent and do daily tasks.
- Major neurocognitive disorder - decreased mental function and loss of ability to do daily tasks. Also called dementia.
Causes
Listed below are conditions associated with neurocognitive disorder.
BRAIN INJURY CAUSED BY TRAUMA
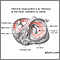
- Bleeding into the brain (intracerebral hemorrhage)
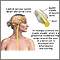
- Bleeding into the space around the brain (subarachnoid hemorrhage)
- Blood clot inside the skull but outside the brain and its covering, which may cause pressure on the brain (subdural or epidural hematoma)
- Concussion
BREATHING CONDITIONS
- Low oxygen in the body (hypoxia)
- High carbon dioxide level in the body (hypercapnia)
CARDIOVASCULAR DISORDERS
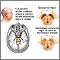
- Dementia due to many strokes (multi-infarct dementia)
- Heart infections (endocarditis, myocarditis)
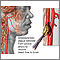
- Stroke
- Transient ischemic attack (TIA)
DEGENERATIVE DISORDERS
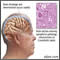
- Alzheimer disease (also called senile dementia, Alzheimer type)
- Creutzfeldt-Jakob disease
- Diffuse Lewy body disease
- Huntington disease
- Multiple sclerosis
- Normal pressure hydrocephalus
- Parkinson disease
- Pick disease
DEMENTIA DUE TO METABOLIC CAUSES
- Kidney disease
- Liver disease
- Thyroid disease (hyperthyroidism or hypothyroidism)
- Vitamin deficiency (B1, B12, or folate)
DRUG AND ALCOHOL-RELATED CONDITIONS
- Alcohol withdrawal state
- Intoxication from drug or alcohol use
- Medicine effect, such as corticosteroids, sedative-hypnotics, antihistamines, and antidepressants
- Wernicke-Korsakoff syndrome, a long-term effect of deficiency of thiamine (vitamin B1)
- Withdrawal from drugs, such as sedative-hypnotics and corticosteroids
INFECTIONS
- Any sudden onset (acute) or long-term (chronic) infection
- Blood poisoning (septicemia)
- Brain infection (encephalitis)
- Meningitis (infection of the lining of the brain and spinal cord)
- Prion infections, such as mad cow disease
- Late-stage syphilis
Complications of cancer and cancer treatment with chemotherapy can also lead to neurocognitive disorder.
Other conditions that may mimic organic brain syndrome include:
- Depression
- Neurosis
- Psychosis
Symptoms
Symptoms can differ based on the disease. In general, organic brain syndrome causes:
- Agitation
- Confusion
- Long-term loss of brain function (dementia)
- Severe, short-term loss of brain function (delirium)
Exams and Tests
Tests depend on the disorder, but may include:
- Blood tests
- Neuropsychological testing
- Electroencephalogram (EEG)
- Head CT scan
- Head MRI
- Lumbar puncture (spinal tap)
Treatment
Treatment depends on the underlying condition. Many conditions are treated mainly with rehabilitation and supportive care to help the person with activities lost due to areas where brain function is affected.
Medicines may be needed to reduce aggressive behaviors that can occur with some of the conditions.
Outlook (Prognosis)
Some disorders are short-term and reversible. But many are long-term or get worse over time.
Possible Complications
People with neurocognitive disorder often lose the ability to interact with others or function on their own.
When to Contact a Medical Professional
Contact your health care provider if:
- You have been diagnosed with organic brain syndrome and you are uncertain about the exact disorder.
- You have symptoms of this condition.
- You have been diagnosed with neurocognitive disorder and your symptoms become worse.
References
Beck BJ, Tompkins KJ. Mental disorders due to another medical condition. In: Stern TA, Fava M, Wilens TE, Rosenbaum JF, eds. Massachusetts General Hospital Comprehensive Clinical Psychiatry. 2nd ed. Philadelphia, PA: Elsevier; 2016:chap 21.
Fernandez-Robles C, Greenberg DB, Pirl WF. Psycho-oncology: Psychiatric co-morbidities and complications of cancer and cancer treatment. In: Stern TA, Fava M, Wilens TE, Rosenbaum JF, eds. Massachusetts General Hospital Comprehensive Clinical Psychiatry. 2nd ed. Philadelphia, PA: Elsevier; 2016:chap 56.
Merrick ST, Jones S, Glesby MJ. Systemic manifestations of HIV/AIDS. In: Goldman L, Schafer AI, eds. Goldman-Cecil Medicine. 26th ed. Philadelphia, PA: Elsevier; 2020:chap 366.
Review Date: 1/23/2022
Reviewed By: Joseph V. Campellone, MD, Department of Neurology, Cooper Medical School at Rowan University, Camden, NJ. Review provided by VeriMed Healthcare Network. Also reviewed by David Zieve, MD, MHA, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.