Meniere disease
Hydrops; Hearing loss; Endolymphatic hydrops; Dizziness - Ménière disease; Vertigo - Ménière disease; Hearing loss - Ménière disease; Overpressure therapy - Ménière disease; Ménière disease
Ménière disease is an inner ear disorder that affects balance and hearing.
Causes
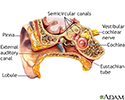
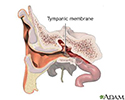
Your inner ear contains fluid-filled tubes called labyrinths. These tubes, along with a nerve in your skull, help you know the position of your body and help maintain your balance.
The exact cause of Ménière disease is unknown. It may occur when the pressure of the fluid in part of the inner ear gets too high.
In some cases, Ménière disease may be related to:
- Head injury
- Middle or inner ear infection
Other risk factors include:
- Alcohol use
- Allergies
- Family history
- Recent cold or viral illness
- Smoking
- Stress
- Use of certain medicines
Ménière disease is a fairly common disorder.
Symptoms
Attacks of Ménière disease often start without warning. They may occur daily or as rarely as once a year. The severity of each attack can vary. Some attacks may be severe and interfere with daily living activities.
Ménière disease usually has four main symptoms:
- Hearing loss that changes
- Pressure in the ear
- Ringing or roaring in the affected ear, called tinnitus
- Vertigo, or dizziness
Severe vertigo is the symptom that causes the most problems. With vertigo, you feel as though you are spinning or moving, or that the world is spinning around you.
- Nausea, vomiting, and sweating often occur.
- Symptoms get worse with sudden movement.
- Often, you will need to lie down and close your eyes.
- You may feel dizzy and off-balance for anywhere from 20 minutes to 24 hours.
Hearing loss is often only in one ear, but it may affect both ears.
- Hearing tends to improve between attacks, but gets worse over time.
- Low frequency hearing is lost first.
- You also may have roaring or ringing in the ear (tinnitus), along with a sense of pressure in your ear
Other symptoms include:
- Diarrhea
- Headaches
- Pain or discomfort in the abdomen
- Nausea and vomiting
- Uncontrollable eye movements (a symptom called nystagmus)
Sometimes the nausea, vomiting, and diarrhea are severe enough that you need to be admitted to the hospital to receive IV fluids or you need to rest at home.
Exams and Tests
A brain and nervous system exam may show problems with hearing, balance, or eye movement.
A hearing test will show the hearing loss that occurs with Ménière disease. Hearing may be near normal after an attack.
A caloric stimulation test checks your eye reflexes by warming and cooling the inner ear with water. Test results that are not in the normal range can be a sign of Ménière disease.
These tests may also be done to check for other causes of vertigo:
- Electrocochleography (ECOG)
- Electronystagmography (ENG) or videonystagmography (VNG)
- Head MRI scan
Treatment
There is no known cure for Ménière disease. However, lifestyle changes and some treatments can help relieve symptoms.
Your health care provider may suggest ways to reduce the amount of fluid in your body. This can often help control symptoms.
- Water pills (diuretics) may help relieve fluid pressure in the inner ear
- A low-salt diet may also help
To help ease symptoms and stay safe:
- Avoid sudden movements, which may worsen symptoms. You may need help walking during attacks.
- Avoid bright lights, TV, and reading during attacks. They can make symptoms worse.
- Do not drive, operate heavy machinery, or climb until 1 week after your symptoms disappear. A sudden dizzy spell during these activities can be dangerous.
- Remain still and rest when you have symptoms.
- Gradually increase your activity after attacks.
Symptoms of Ménière disease can cause stress. Make healthy lifestyle choices to help you cope:
- Eat a well-balanced, healthy diet. Don't overeat.
- Exercise regularly, if possible.
- Get enough sleep.
- Limit caffeine and alcohol.
Help ease stress by using relaxation techniques, such as:
- Guided imagery
- Meditation
- Progressive muscle relaxation
- Tai chi
- Yoga
Ask your provider about other self-care measures.
Your provider may prescribe:
- Antinausea medicines to relieve nausea and vomiting
- Diazepam (Valium) or motion sickness medicines, such as meclizine (Antivert, Bonine, Dramamine) to relieve dizziness and vertigo
Other treatments that may be helpful include:
- A hearing aid to improve hearing in the affected ear.
- Balance therapy, which includes head, eye, and body exercises you can do at home to help train your brain to overcome dizziness.
- Overpressure therapy using a device that sends tiny pressure pulses through the ear canal to the middle ear. The pulses are aimed reducing amount of fluid in the middle ear, which in turn reduces dizziness.
You may need ear surgery if your symptoms are severe and do not respond to other treatments.
- Surgery to cut the vestibular nerve helps control vertigo. It does not damage hearing.
- Surgery to decompress a structure in the inner ear called the endolymphatic sac. Hearing may be affected by this procedure.
- Injecting steroids or an antibiotic called gentamicin directly into the middle ear can help control vertigo.
- Removing part of the inner ear (labyrinthectomy) helps treat vertigo. This causes complete hearing loss.
Support Groups
These resources can provide more information on Ménière disease:
- American Academy of Otolaryngology-Head and Neck Surgery -- www.enthealth.org/conditions/menieres-disease/
- National Institute on Deafness and Other Communication Disorders -- www.nidcd.nih.gov/health/menieres-disease
- Vestibular Disorders Association -- vestibular.org/menieres-disease
Outlook (Prognosis)
Ménière disease can often be controlled with treatment. Or, the condition may get better on its own. In some cases, Ménière disease can be chronic (long-term) or disabling.
When to Contact a Medical Professional
Call your provider if you have symptoms of Ménière disease, or if symptoms get worse. These include hearing loss, ringing in the ears, or dizziness.
Prevention
You can't prevent Ménière disease. Treating early symptoms right away may help prevent the condition from getting worse. Treating an ear infection and other related disorders may be helpful.
References
Boomsaad ZE, Telian SA, Patil PG. Treatment of intractable vertigo. In: Winn HR, ed. Youmans and Winn Neurological Surgery. 7th ed. Philadelphia, PA: Elsevier; 2017:chap 105.
Crane BT, Minor LB. Peripheral vestibular disorders. In: Flint PW, Haughey BH, Francis HW, et al, eds. Cummings Otolaryngology: Head and Neck Surgery. 7th ed. Philadelphia, PA: Elsevier; 2021:chap 167.
National Institute on Deafness and Other Communicable Diseases website. Meniere's disease. www.nidcd.nih.gov/health/menieres-disease. Updated February 13, 2017. Accessed November 30, 2021.
Review Date: 7/26/2021
Reviewed By: Joseph V. Campellone, MD, Department of Neurology, Cooper Medical School at Rowan University, Camden, NJ. Review provided by VeriMed Healthcare Network. Also reviewed by David Zieve, MD, MHA, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.