Secondary systemic amyloidosis
Amyloidosis - secondary systemic; AA amyloidosis
Secondary systemic amyloidosis is a disorder in which abnormal proteins build up in tissues and organs. Clumps of the abnormal proteins are called amyloid deposits.
Secondary means it occurs because of another disease or situation. For example, this condition usually occurs due to long-term (chronic) infection or inflammation. In contrast, primary amyloidosis means there is no other disease that is causing the condition.
Systemic means that the disease affects the entire body.
Causes
The exact cause of secondary systemic amyloidosis is unknown. You are more likely to develop secondary systemic amyloidosis if you have a long-term infection or inflammation.
This condition may occur with:
- Ankylosing spondylitis -- a form of arthritis that mostly affects the bones and joints in the spine
- Bronchiectasis -- disease in which the large airways in the lungs are damaged by chronic infection
- Chronic osteomyelitis -- bone infection
- Cystic fibrosis -- a genetic disease that causes thick, sticky mucus to build up in the lungs, digestive tract, and other areas of the body, leading to chronic infection of the lungs
- Familial Mediterranean fever -- inherited disorder of repeated fevers and inflammation that often affects the lining of the abdomen, chest, or joints
- Gout
- Hairy cell leukemia -- a type of blood cancer
- Hodgkin disease -- cancer of the lymph tissue
- Inflammatory bowel disease
- Juvenile idiopathic arthritis -- arthritis that affects children
- Multiple myeloma -- a type of blood cancer
- Psoriatic arthritis
- Reactive arthritis -- a group of conditions that causes swelling and inflammation of the joints, eyes, and urinary and genital systems)
- Rheumatoid arthritis
- Systemic lupus erythematosus -- an autoimmune disorder
- Tuberculosis
- Vasculitis (inflammation of the blood vessels)
Symptoms
Symptoms of secondary systemic amyloidosis depend on which body tissue is affected by the protein deposits. These deposits damage normal tissues. This may lead to the symptoms or signs of this illness, including:
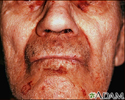
- Bleeding in the skin
- Fatigue
- Irregular heartbeat
- Numbness of hands and feet
- Rash
- Shortness of breath
- Swallowing difficulties
- Swollen arms or legs
- Swollen tongue
- Weak hand grip
- Weight loss
Exams and Tests
The health care provider will perform a physical examination and ask about your symptoms.
Tests that may be done include:
- Abdominal ultrasound (may show a swollen liver or spleen)
- Biopsy or aspiration of fat just beneath the skin (subcutaneous fat)
- Biopsy of rectum
- Biopsy of skin
- Biopsy of bone marrow
- Blood tests, including creatinine and BUN (blood urea nitrogen)
- Echocardiogram
- Electrocardiogram (ECG)
- Nerve conduction velocity
- Urinalysis
Treatment
The condition that is causing the amyloidosis should be treated. In some cases, the drug colchicine or an immunosuppressive drug (medicine that treats the immune system) is prescribed.
Outlook (Prognosis)
How well a person does depends on which organs are affected. It also depends on, whether the disease that is causing it can be controlled. If the disease involves the heart and kidneys, it may lead to organ failure and death.
Possible Complications
Health problems that may result from secondary systemic amyloidosis include:
- Endocrine failure
- Heart failure
- Kidney failure
- Respiratory failure
When to Contact a Medical Professional
Call your provider if you have symptoms of this condition. The following are serious symptoms that need prompt medical attention:
- Bleeding
- Irregular heartbeat
- Numbness
- Shortness of breath
- Swelling
- Weak grip
Prevention
If you have a disease that is known to increase your risk for this condition, make sure you get it treated. This may help prevent amyloidosis.
References
Gertz MA. Amyloidosis. In: Goldman L, Schafer AI, eds. Goldman-Cecil Medicine. 26th ed. Philadelphia, PA: Elsevier; 2020:chap 179.
Papa R, Lachmann HJ. Secondary, AA, amyloidosis. Rheum Dis Clin North Am. 2018;44(4):585-603. PMID: 30274625 pubmed.ncbi.nlm.nih.gov/30274625/.
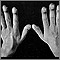
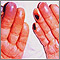
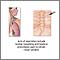
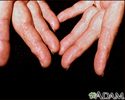
Amyloidosis of the fingers - illustration
Amyloidosis of the fingers
illustration
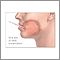
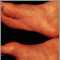
Amyloidosis of the face - illustration
Amyloidosis of the face
illustration
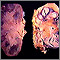
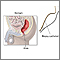
Antibodies - illustration
Antibodies
illustration
Review Date: 4/24/2021
Reviewed By: David C. Dugdale, III, MD, Professor of Medicine, Division of General Medicine, Department of Medicine, University of Washington School of Medicine. Also reviewed by David Zieve, MD, MHA, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.