Granulomatosis with polyangiitis
Formerly: Wegener's granulomatosis
Granulomatosis with polyangiitis (GPA) is a rare disorder in which blood vessels become inflamed. This leads to damage in major organs of the body. It was formerly known as Wegener's granulomatosis.
Causes
GPA mainly causes inflammation of blood vessels in the lungs, kidneys, nose, sinuses, and ears. This is called vasculitis or angiitis. Other areas may also be affected in some cases. The disease can be fatal and prompt treatment is important.
In most cases, the exact cause is not known, but it is an autoimmune disorder. Rarely, vasculitis with positive antineutrophil cytoplasmic antibodies (ANCA) has been caused by several drugs including cocaine cut with levamisole, hydralazine, propylthiouracil, and minocycline.
GPA is most common in middle-aged adults of northern European descent. It is rare in children.
Symptoms
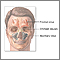
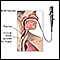
Frequent sinusitis and bloody noses are the most common symptoms. Other early symptoms include a fever that has no clear cause, night sweats, fatigue, and a general ill feeling (malaise).
Other common symptoms may include:
- Chronic ear infections
- Pain, and sores around the opening of the nose
- Cough with or without blood in the sputum
- Chest pain and shortness of breath as the disease progresses
- Loss of appetite and weight loss
- Skin changes such as bruises and ulcers of the skin
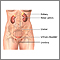
- Kidney problems
- Bloody urine
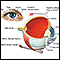
- Eye problems ranging from mild conjunctivitis to severe swelling of the eye
Less common symptoms include:
- Joint pain
- Weakness
- Abdominal pain
Exams and Tests
You may have a blood test that looks for ANCA proteins. These tests are done in most people with active GPA. However, this test is sometimes negative, even in people with the condition.
A chest x-ray will be done to look for signs of lung disease.
Urinalysis is done to look for signs of kidney disease such as protein and blood in the urine. Sometimes urine is collected over 24 hours to check how the kidneys are working.
Standard blood tests include:
- Complete blood count (CBC)
- Comprehensive metabolic panel
- Erythrocyte sedimentation rate (ESR)
Blood tests may be done to exclude other illnesses. These may include:
- Antinuclear antibodies
- Anti-glomerular basement membrane (anti-GBM) antibodies
- C3 and C4, cryoglobulins, hepatitis serologies, HIV
- Liver function tests
- Tuberculosis screen and blood cultures
A biopsy is sometimes needed to confirm the diagnosis and check how severe the disease is. A kidney biopsy is most commonly done. You may also have one of the following:
Other tests that may be done include:
- Sinus CT scan
- Chest CT scan
Treatment
Because of the potentially serious nature of GPA, you may be hospitalized. Once the diagnosis is made, you will probably be treated with high doses of glucocorticoids (such as prednisone). These are given through the vein for 3 to 5 days at the beginning of treatment. Prednisone is given along with other medicines that slow down the immune response.
For milder disease other medicines that slow down the immune response such as methotrexate or azathioprine may be used.
Common medicines for vasculitis include:
- Rituximab (Rituxan)
- Cyclophosphamide (Cytoxan)
- Methotrexate
- Azathioprine (Imuran)
- Mycophenolate (Cellcept or Myfortic)
These medicines are effective in severe disease, but they may cause serious side effects. Most people with GPA are treated with ongoing medicines to prevent relapse for at least 12 to 24 months. Talk to your health care provider about your treatment plan.
Other medicines used for GPA include:
- Medicines to prevent bone loss caused by prednisone
- Folic acid or folinic acid, if you are taking methotrexate
- Antibiotics to prevent lung infections
Support Groups
Support groups with others who suffer from similar diseases may help people with the condition and their families learn about the diseases and adjust to the changes associated with the treatment.
Outlook (Prognosis)
Without treatment, people with severe forms of this disease can die within a few months.
With treatment, the outlook for most patients is good. Most people who receive corticosteroids and other medicines that slow the immune response get much better. Most people with GPA are treated with ongoing medicines to prevent relapse for at least 12 to 24 months.
Possible Complications
Complications most often occur when the disease is not treated. People with GPA develop tissue damage in the lungs, airways, and the kidneys. Kidney involvement may result in blood in the urine and kidney failure. Kidney disease can quickly get worse. Kidney function may not improve even when the condition is controlled by medicines.
If untreated, kidney failure and possibly death occur in most cases.
Other complications may include:
- Eye swelling
- Lung failure
- Coughing up blood
- Nasal septum perforation (hole inside the nose)
- Side effects from medicines used to treat the disease
When to Contact a Medical Professional
Call your provider if:
- You develop chest pain and shortness of breath.
- You cough up blood.
- You have blood in your urine.
- You have other symptoms of this disorder.
Prevention
There is no known prevention.
References
Grau RG. Drug-induced vasculitis: New insights and a changing lineup of suspect. Curr Rheumatol Rep. 2015;17(12):71. PMID: 26503355 pubmed.ncbi.nlm.nih.gov/26503355/.
Pagnoux C, Guillevin L; French Vasculitis Study Group; MAINRITSAN investigators. Rituximab or azathioprine maintenance in ANCA-associated vasculitis. N Engl J Med. 2015;372(4):386-387. PMID: 25607433 pubmed.ncbi.nlm.nih.gov/25607433/.
Stone JH. The systemic vasculitides. In: Goldman L, Schafer AI, eds. Goldman-Cecil Medicine. 26th ed. Philadelphia, PA: Elsevier; 2020:chap 254.
Yates M, Watts RA, Bajema IM, et al. EULAR/ERA-EDTA recommendations for the management of ANCA-associated vasculitis. [published correction appears in Ann Rheum Dis. 2017;76(8):1480]. Ann Rheum Dis. 2016;75(9):1583-1594. PMID: 27338776 pubmed.ncbi.nlm.nih.gov/27338776/.
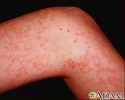
Granulomatosis with polyangiitis on the leg - illustration
Granulomatosis with polyangiitis on the leg
illustration
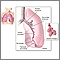
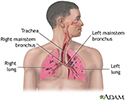
Respiratory system - illustration
Respiratory system
illustration
Review Date: 10/25/2021
Reviewed By: Diane M. Horowitz, MD, Rheumatology and Internal Medicine, Northwell Health, Great Neck, NY. Review provided by VeriMed Healthcare Network. Also reviewed by David Zieve, MD, MHA, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.