Health Library
Transjugular intrahepatic portosystemic shunt (TIPS)
TIPS; Cirrhosis - TIPS; Liver failure - TIPS
Transjugular intrahepatic portosystemic shunt (TIPS) is a procedure to create new connections between two blood vessels in your liver. You may need this procedure if you have severe liver problems.
Images
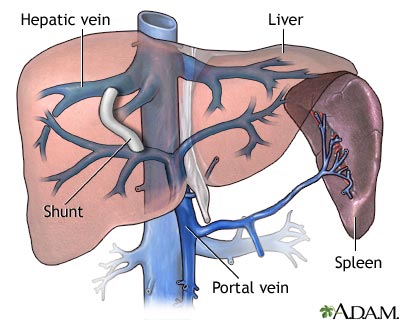
I Would Like to Learn About:
Description
This is not a surgical procedure. It is done by an interventional radiologist using x-ray guidance. A radiologist is a doctor who uses imaging techniques to diagnose and treat diseases.
You will be asked to lie on your back. You will be connected to monitors that will check your heart rate and blood pressure.
You will probably receive local anesthesia and medicine to relax you. This will make you pain-free and sleepy. Or, you may have general anesthesia (asleep and pain-free).
During the procedure:
- The doctor inserts a catheter (a flexible tube) through your skin into a vein in your neck. This vein is called the jugular vein. On the end of the catheter is a tiny balloon and a metal mesh stent (tube).
- Using an x-ray machine, the doctor guides the catheter into a vein in your liver.
- Dye (contrast material) is then injected into the vein so that it can be seen more clearly.
- The balloon is inflated to place the stent. You may feel a little pain when this happens.
- The doctor uses the stent to connect your portal vein to one of your hepatic veins.
- At the end of the procedure, your portal vein pressure is measured to make sure it has gone down.
- The catheter with the balloon is then removed.
- After the procedure, a small bandage is placed over the neck area. There are usually no stitches.
- The procedure takes about 60 to 90 minutes to complete.
This new pathway will allow blood to flow better. It will ease pressure on the veins of your stomach, esophagus, intestines, and liver.
Why the Procedure Is Performed
Normally, blood coming from your esophagus, stomach, and intestines first flows through the liver. When your liver has a lot of damage and there are blockages, blood cannot flow through it very easily. This is called portal hypertension (increased pressure and backup of the portal vein). The veins can then break open (rupture), causing serious bleeding.
Common causes of portal hypertension are:
- Alcohol use causing scarring of the liver (cirrhosis)
- Blood clots in a vein that flows from the liver to the heart
- Too much iron in the liver (hemochromatosis)
- Hepatitis B or hepatitis C
When portal hypertension occurs, you may have:
- Bleeding from veins of the stomach, esophagus, or intestines (variceal bleeding)
- Buildup of fluid in the belly (ascites)
- Buildup of fluid in the chest (hydrothorax)
This procedure allows blood to flow better in your liver, stomach, esophagus, and intestines, and then back to your heart.
Risks
Possible risks with this procedure are:
- Damage to blood vessels
- Fever
- Hepatic encephalopathy (a disorder that affects concentration, mental function, and memory, and may lead to coma)
- Infection, bruising, or bleeding
- Reactions to medicines or the dye
- Stiffness, bruising, or soreness in the neck
Rare risks are:
- Bleeding in the belly
- Blockage in the stent
- Cutting of blood vessels in the liver
- Heart problems or abnormal heart rhythms
- Infection of the stent
Before the Procedure
Your doctor may ask you to have these tests:
- Blood tests (complete blood count, electrolytes, and kidney tests)
- Chest x-ray or ECG
Tell your health care provider:
- If you are or could be pregnant
- Any medicines you are taking, even drugs, supplements, or herbs you bought without a prescription (your doctor may ask you to stop taking blood thinners like aspirin, heparin, warfarin, or other blood thinners a few days before the procedure)
On the day of your procedure:
- Follow instructions on when to stop eating and drinking before the procedure.
- Ask your doctor which medicines you should still take on the day of the procedure. Take these drugs with a small sip of water.
- Follow instructions on taking a shower before the procedure.
- Arrive on time at the hospital.
- You should plan to stay overnight at the hospital.
After the Procedure
After the procedure, you will recover in your hospital room. You will be monitored for bleeding. You will have to keep your head raised.
There is usually no pain after the procedure.
You will be able to go home when you feel better. This may be the day after the procedure.
Many people get back to their everyday activities in 7 to 10 days.
Your doctor will probably do an ultrasound after the procedure to make sure the stent is working correctly.
You will be asked to have a repeat ultrasound in a few weeks to make sure that the TIPS procedure is working.
Outlook (Prognosis)
Your radiologist can tell you right away how well the procedure worked. Most people recover well.
TIPS works in about 80% to 90% of portal hypertension cases.
The procedure is much safer than surgery and does not involve any cutting or stitches.
Related Information
Hepatic vein obstruction (Budd-Chiari)Cirrhosis
Alcoholic liver disease
Ascites
Loss of brain function - liver disease
Portacaval shunting
Stent
Cirrhosis - discharge
References
Darcy MD. Transjugular intrahepatic portosystemic shunting: indications and technique. In: Jarnagin WR, ed. Blumgart's Surgery of the Liver, Biliary Tract, and Pancreas. 6th ed. Philadelphia, PA: Elsevier; 2017:chap 87.
Dariushnia SR, Haskal ZJ, Midia M, et al. Quality improvement guidelines for transjugular intrahepatic portosystemic shunts. J Vasc Interv Radiol. 2016;27(1):1-7. PMID: 26614596 pubmed.ncbi.nlm.nih.gov/26614596/.
Liddell RP, Transjugular intrahepatic portosystemic shunting. In: Cameron AM, Cameron JL, eds. Current Surgical Therapy. 13th ed. Philadelphia, PA: Elsevier; 2020:417-424.
BACK TO TOPReview Date: 1/15/2021
Reviewed By: Michael M. Phillips, MD, Emeritus Professor of Medicine, The George Washington University School of Medicine, Washington, DC. Also reviewed by David Zieve, MD, MHA, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.
 | A.D.A.M., Inc. is accredited by URAC, for Health Content Provider (www.urac.org). URAC's accreditation program is an independent audit to verify that A.D.A.M. follows rigorous standards of quality and accountability. A.D.A.M. is among the first to achieve this important distinction for online health information and services. Learn more about A.D.A.M.'s editorial policy, editorial process and privacy policy. A.D.A.M. is also a founding member of Hi-Ethics. This site complies with the HONcode standard for trustworthy health information: verify here. |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. © 1997- 2021 A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited.
