Health Library
Chest MRI
Nuclear magnetic resonance - chest; Magnetic resonance imaging - chest; NMR - chest; MRI of the thorax; Thoracic MRI
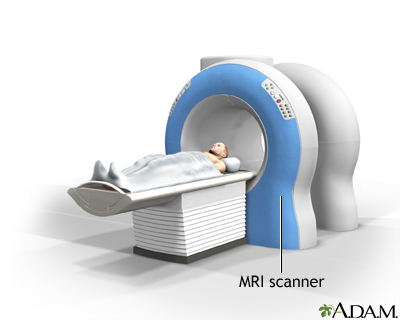
A chest MRI (magnetic resonance imaging) scan is an imaging test that uses powerful magnetic fields and radio waves to create pictures of the chest (thoracic area). It does not use radiation (x-rays).
Images
I Would Like to Learn About:
How the Test is Performed
The test is done in the following way:
- You may be asked to wear a hospital gown or clothing without metal fasteners (such as sweatpants and a t-shirt). Certain types of metal can cause blurry images or be dangerous to have on in the scanner room.
- You lie on a narrow table, which slides into the large tunnel-shaped scanner.
- You must be still during the exam, because movement causes blurred images. You may be told to hold your breath for short periods.
Some exams require a special dye called contrast. The dye is usually given before the test through a vein (IV) in your hand or forearm. The dye helps the radiologist see certain areas more clearly. A blood test to measure your kidney function may be done before the test. This is to make sure your kidneys are healthy enough to filter the contrast.
During the MRI, the person who operates the machine will watch you from another room. The test most often lasts 30 to 60 minutes, but it may take longer.
How to Prepare for the Test
You may be asked not to eat or drink anything for 4 to 6 hours before the scan.
Tell your provider if you are claustrophobic (afraid of closed spaces). You may be given a medicine to help you feel sleepy and less anxious. Your provider may suggest an "open" MRI, in which the machine is not as close to your body.
Before the test, tell your health care provider if you have:
- Brain aneurysm clips
- Artificial heart valves
- Heart defibrillator or pacemaker
- Inner ear (cochlear) implants
- Kidney disease or are on dialysis (you may not be able to receive contrast)
- Recently placed artificial joints
- Vascular stents
- Worked with sheet metal in the past (you may need tests to check for metal pieces in your eyes)
The MRI contains strong magnets, so metal objects are not allowed into the room with the MRI scanner. This is because there is a risk that they will be drawn from your body toward the scanner. Examples of metal objects you will need to remove are:
- Pens, pocket knives, and eyeglasses
- Items such as jewelry, watches, credit cards, and hearing aids
- Pins, hairpins, and metal zippers
- Removable dental work
Some of the newer medical devices described above are MRI compatible, so the radiologist needs to check the device manufacturer to determine if an MRI is possible.
How the Test will Feel
An MRI exam causes no pain. If you have trouble lying still or are very nervous, you may be given medicine to relax. Too much movement can blur MRI images and cause errors when the doctor looks at the images.
The table may be hard or cold, but you can ask for a blanket or pillow. The machine produces loud thumping and humming noises when turned on. You can wear ear plugs to help reduce the noise.
An intercom in the room allows you to speak to someone at any time. Some MRIs have televisions and special headphones that you can use to help the time pass.
There is no recovery time, unless you were given a medicine to relax. After an MRI scan, you can resume your normal diet, activity, and medicines.
Why the Test is Performed
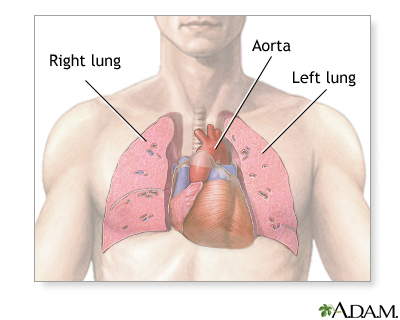
A chest MRI provides detailed pictures of tissues within the chest area. In general, it is not as good at looking at the lungs as a CT chest scan, but it can be better for other tissues.
A chest MRI may be done to:
- Provide an alternative to angiography, or avoid repeated exposure to radiation
- Clarify findings from earlier x-rays or CT scans
- Diagnose abnormal growths in the chest
- Evaluate blood flow
- Show lymph nodes and blood vessels
- Show the structures of the chest from many angles
- See if cancer in the chest has spread to other areas of the body (this is called staging -- it helps guide future treatment and follow-up, and gives you an idea of what to expect in the future)
- Detect tumors, especially in the middle part of the chest (mediastinum)
Normal Results
A normal result means your chest area appears normal.
What Abnormal Results Mean
An abnormal chest MRI may be due to:
- A tear in the wall, an abnormal widening or ballooning, or narrowing of the major artery carrying blood out of the heart (aorta)
- Other abnormal changes of the major blood vessels in the lungs or chest
- Buildup of blood or fluid around the heart (pericardial effusion) or the lungs (pleural effusion)
- Lung cancer or cancer that has spread to the lungs from elsewhere in the body
- Cancer or tumors of the heart
- Cancer or tumors of the chest, such as a thymus tumor
- Disease in which the heart muscle becomes weakened, stretched, or has another structural problem (cardiomyopathy)
- Damage to, and widening of the large airways of the lungs (bronchiectasis)
- Enlarged lymph nodes
- Infection of the heart tissue or heart valve
- Esophageal cancer
- Lymphoma in the chest
- Birth defects of the heart
- Tumors, nodules, or cysts in the chest
Risks
MRI uses no radiation. To date, no side effects from the magnetic fields and radio waves have been reported.
The most common type of contrast (dye) used is gadolinium. It is very safe. Allergic reactions to the substance rarely occur. However, gadolinium can be harmful to people with kidney problems who need dialysis. If you have kidney problems, tell your provider before the test.
The strong magnetic fields created during an MRI can cause heart pacemakers and other implants not to work as well. It can also cause a piece of metal inside your body to move or shift.
Considerations
Currently, MRI is not considered a valuable tool for spotting or monitoring slight changes in lung tissue. The lungs contain mostly air and are hard to image. CT scan tends to be better for monitoring these changes.
Disadvantages of MRI include:
- High cost
- Long length of the scan
- Sensitivity to movement
Related Information
MRICT scan
Arteriogram
Lymphofollicular hyperplasia
Swollen lymph nodes
Chronic obstructive pulmonary disease (COPD)
Bronchiectasis
Cystic fibrosis
Pleural effusion
Coarctation of the aorta
Aortic stenosis
Aortic dissection
Pericarditis
Thoracic aortic aneurysm
Atrial septal defect (ASD)
Cardiac tamponade
Mitral valve prolapse
Pulmonary edema
Restrictive cardiomyopathy
SVC obstruction
Abdominal aortic aneurysm repair - open - discharge
References
Ackman JB. Thoracic magnetic resonance imaging: technique and approach to diagnosis. In: Shephard J-AO, ed. Thoracic Imaging: The Requisites. 3rd ed. Philadelphia, PA: Elsevier; 2019:chap 3.
Jokerst CE, Gotway MB. Thoracic radiology: noninvasive diagnostic imaging. In: Broaddus VC, Ernst JD, King TE, et al, eds. Murray and Nadel's Textbook of Respiratory Medicine. 7th ed. Philadelphia, PA: Elsevier; 2022:chap 20.
BACK TO TOPReview Date: 7/31/2022
Reviewed By: Denis Hadjiliadis, MD, MHS, Paul F. Harron, Jr. Professor of Medicine, Pulmonary, Allergy, and Critical Care, Perelman School of Medicine, University of Pennsylvania, Philadelphia, PA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.
 | A.D.A.M., Inc. is accredited by URAC, for Health Content Provider (www.urac.org). URAC's accreditation program is an independent audit to verify that A.D.A.M. follows rigorous standards of quality and accountability. A.D.A.M. is among the first to achieve this important distinction for online health information and services. Learn more about A.D.A.M.'s editorial policy, editorial process and privacy policy. A.D.A.M. is also a founding member of Hi-Ethics. This site complies with the HONcode standard for trustworthy health information: verify here. |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. © 1997- 2023 A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited.
