Health Library
CEA blood test
Carcinoembryonic antigen blood test
The carcinoembryonic antigen (CEA) test measures the level of CEA in the blood. CEA is a protein normally found in the tissue of a developing baby in the womb. The blood level of this protein disappears or becomes very low after birth. In adults, an abnormal level of CEA may be a sign of cancer.
Images
I Would Like to Learn About:
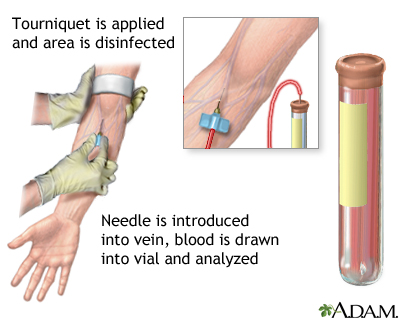
How the Test is Performed
How to Prepare for the Test
Smoking may increase the CEA level. If you smoke, your health care provider may tell you to avoid doing so for a short time before the test.
How the Test will Feel
When the needle is inserted to draw blood, some people feel moderate pain. Others feel only a prick or stinging. Afterward, there may be some throbbing or a slight bruise. This soon goes away.
Why the Test is Performed
This test is done to monitor the response to treatment and then to check for the return of colon and other cancers such as medullary thyroid cancer and cancers of the rectum, lung, breast, liver, pancreas, stomach, and ovaries.
It is not used as a screening test for cancer and should not be done unless a diagnosis of cancer has been made.
Normal Results
The normal range is 0 to 2.5 ng/mL (0 to 2.5 µg/L).
In smokers, slightly higher values may be considered normal (0 to 5 ng/mL, or 0 to 5 µg/L).
What Abnormal Results Mean
A high CEA level in a person recently treated for certain cancers may mean the cancer has returned. A higher than normal level may be due to the following cancers:
- Breast cancer
- Cancers of the reproductive and urinary tracts
- Colon cancer
- Lung cancer
- Pancreatic cancer
- Thyroid cancer
Higher than normal CEA level alone cannot diagnose a new cancer. Further testing is needed.
An increased CEA level may also be due to:
- Liver and gallbladder problems, such as scarring of the liver (cirrhosis), or gallbladder inflammation (cholecystitis)
- Heavy smoking
- Inflammatory bowel diseases (such as ulcerative colitis or diverticulitis)
- Lung infection
- Inflammation of the pancreas (pancreatitis)
- Stomach ulcer
Risks
There is little risk involved with having your blood taken. Veins and arteries vary in size from one person to another and from one side of the body to the other. Taking blood from some people may be more difficult than from others.
Other risks associated with having blood drawn are slight but may include:
- Excessive bleeding (rare)
- Fainting or feeling lightheaded
- Multiple punctures to locate veins
- Hematoma (blood accumulating under the skin)
- Infection (a slight risk any time the skin is broken)
Related Information
Protein in dietColorectal cancer
Cancer
Breast cancer
Lung cancer - small cell
Pancreatic cancer
Thyroid cancer
Ulcerative colitis
Diverticulitis
Acute cholecystitis
Cirrhosis
Liver disease
Peptic ulcer
Pulmonary angiography
References
Franklin WA, Aisner DL, Davies KD, et al. Pathology, biomarkers, and molecular diagnostics. In: Niederhuber JE, Armitage JO, Kastan MB, Doroshow JH, Tepper JE, eds. Abeloff's Clinical Oncology. 6th ed. Philadelphia, PA: Elsevier; 2020:chap 15.
Lee P, Jain S, Pincus WR, Khalili M, Bowne WB, Bluth MH, McPherson RA. Diagnosis and management of cancer using serologic and other body fluid markers. In: McPherson RA, Pincus MR, eds. Henry's Clinical Diagnosis and Management by Laboratory Methods. 24th ed. Philadelphia, PA: Elsevier; 2022:chap 76.
BACK TO TOPReview Date: 7/19/2021
Reviewed By: Todd Gersten, MD, Hematology/Oncology, Florida Cancer Specialists & Research Institute, Wellington, FL. Review provided by VeriMed Healthcare Network. Also reviewed by David Zieve, MD, MHA, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.
 | A.D.A.M., Inc. is accredited by URAC, for Health Content Provider (www.urac.org). URAC's accreditation program is an independent audit to verify that A.D.A.M. follows rigorous standards of quality and accountability. A.D.A.M. is among the first to achieve this important distinction for online health information and services. Learn more about A.D.A.M.'s editorial policy, editorial process and privacy policy. A.D.A.M. is also a founding member of Hi-Ethics. This site complies with the HONcode standard for trustworthy health information: verify here. |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. © 1997- 2022 A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited.
