Health Library
Spleen removal
Splenectomy; Laparoscopic splenectomy; Spleen removal - laparoscopic
Spleen removal is surgery to remove a diseased or damaged spleen. This surgery is called splenectomy.
The spleen is in the upper part of the belly, on the left side underneath the ribcage. The spleen helps the body fight germs and infections. It also helps filter the blood.
Images
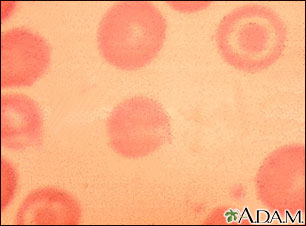
Presentation
I Would Like to Learn About:
Description
The spleen is removed while you are under general anesthesia (asleep and pain-free). The surgeon may do either an open splenectomy or a laparoscopic splenectomy.
During open spleen removal:
- The surgeon makes a cut (incision) in the middle of the belly or on the left side of the belly just below the ribs.
- The spleen is located and removed.
- If you are also being treated for cancer, lymph nodes in the belly are examined. They may also be removed.
- The incision is closed using stitches or staples.
During laparoscopic spleen removal:
- The surgeon makes 3 or 4 small cuts in the belly.
- The surgeon inserts an instrument called a laparoscope through one of the cuts. The scope has a tiny camera and light on the end, which allows the surgeon to see inside the belly. Other instruments are inserted through the other cuts.
- A harmless gas is pumped into the belly to expand it. This gives the surgeon room to work.
- The surgeon uses the scope and other instruments to remove the spleen.
- The scope and other instruments are removed. The incisions are closed using stitches or staples.
With laparoscopic surgery, recovery is often faster and less painful than with open surgery. Talk to your surgeon about which type of surgery is right for you or your child.
Why the Procedure Is Performed
Conditions that may require spleen removal include:
- Abscess or cyst in the spleen.
- Blood clot (thrombosis) in the blood vessels of the spleen.
- Cirrhosis of the liver.
- Diseases or disorders of blood cells, such as idiopathic thrombocytopenia purpura (ITP), hereditary spherocytosis, thalassemia, hemolytic anemia, and hereditary elliptocytosis. These are all rare conditions.
- Hypersplenism (overactive spleen).
- Cancer of the lymph system such as Hodgkin disease.
- Leukemia.
- Other tumors or cancers that affect the spleen.
- Sickle cell anemia.
- Splenic artery aneurysm (rare).
- Trauma to the spleen.
Risks
Risks for anesthesia and surgery in general are:
- Reactions to medicines
- Breathing problems
- Bleeding, blood clots, infection
Risks for this surgery include:
- Blood clot in the portal vein (an important vein that carries blood to the liver)
- Collapsed lung
- Hernia at the surgical cut site
- Increased risk for infection after splenectomy (children are at higher risk than adults for infection)
- Injury to nearby organs, such as the pancreas, stomach, and colon
- Pus collection under the diaphragm
Risks are the same for both open and laparoscopic spleen removal.
Before the Procedure
You or your child will have many visits with health care providers and several tests before surgery. You may have:
- A complete physical exam
- Immunizations, such as the pneumococcal, meningococcal, Haemophilus influenzae, and flu vaccines
- Screening blood tests, special imaging tests, and other tests to make sure you are healthy enough to have surgery
- Transfusions to receive extra red blood cells and platelets, if you need them
If you smoke, you should try to stop. Smoking increases your risk for problems such as slow healing. Ask your provider for help quitting.
Tell the provider:
- If you are, or might be pregnant.
- What medicines, vitamins, and other supplements you or your child is taking, even ones that were bought without a prescription.
During the week before surgery:
- You or your child may need to temporarily stop taking blood thinners. These include aspirin, ibuprofen (Advil, Motrin), clopidogrel (Plavix), vitamin E, and warfarin (Coumadin).
- Ask the surgeon which drugs you or your child should still take on the day of surgery.
On the day of surgery:
- Follow instructions about when you or your child should stop eating or drinking.
- Take the drugs the surgeon told you or your child to take with a small sip of water.
- Arrive at the hospital on time.
After the Procedure
You or your child will spend less than a week in the hospital. The hospital stay may be only 1 or 2 days after a laparoscopic splenectomy. Healing will likely take 4 to 6 weeks.
After going home, follow instructions on taking care of yourself or your child.
Outlook (Prognosis)
The outcome of this surgery depends on what disease or injuries you or your child has. People who do not have other severe injuries or medical problems often recover after this surgery.
After the spleen is removed, a person is more likely to develop infections. Talk with your provider about getting needed vaccinations, particularly the yearly flu vaccine. Children may need to take antibiotics to prevent infections. Most adults do not need antibiotics long-term.
Related Information
Immune thrombocytopenic purpura (ITP)Hemolytic anemia
Hereditary spherocytic anemia
Hodgkin lymphoma
Surgical wound care - open
When you have nausea and vomiting
Spleen removal - child - discharge
Laparoscopic spleen removal in adults - discharge
Open spleen removal in adults - discharge
References
Brandow AM, Camitta BM. Hyposplenism, splenic trauma, and splenectomy. In: Kliegman RM, St. Geme JW, Blum NJ, Shah SS, Tasker RC, Wilson KM, eds. Nelson Textbook of Pediatrics. 21st ed. Philadelphia, PA: Elsevier; 2020:chap 514.
Liveris A, Muscarella P. Management of cysts, tumors, and abscesses of the spleen. In: Cameron JL, Cameron AM, eds. Current Surgical Therapy. 13th ed. Philadelphia, PA: Elsevier; 2020:612-616.
Nassar AK, Hawn M. The spleen. In: Townsend CM, Jr, Beauchamp RD, Evers BM, Mattox KL, eds. Sabiston Textbook of Surgery. 21st ed. Philadelphia, PA: Elsevier; 2022:chap 57.
BACK TO TOPReview Date: 3/15/2021
Reviewed By: Debra G. Wechter, MD, FACS, General Surgery Practice Specializing in Breast Cancer, Virginia Mason Medical Center, Seattle, WA. Also reviewed by David Zieve, MD, MHA, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.
 | A.D.A.M., Inc. is accredited by URAC, for Health Content Provider (www.urac.org). URAC's accreditation program is an independent audit to verify that A.D.A.M. follows rigorous standards of quality and accountability. A.D.A.M. is among the first to achieve this important distinction for online health information and services. Learn more about A.D.A.M.'s editorial policy, editorial process and privacy policy. A.D.A.M. is also a founding member of Hi-Ethics. This site complies with the HONcode standard for trustworthy health information: verify here. |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. © 1997- 2021 A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited.
