Health Library
Vertigo-associated disorders
Peripheral vertigo; Central vertigo; Dizziness; Benign positional vertigo; Benign paroxysmal positional vertigo
Vertigo is a sensation of motion or spinning that is often described as dizziness.
Vertigo is not the same as being lightheaded. People with vertigo feel as though they are actually spinning or moving, or that the world is spinning around them.
Images
I Would Like to Learn About:
Causes
There are two types of vertigo, peripheral and central vertigo.
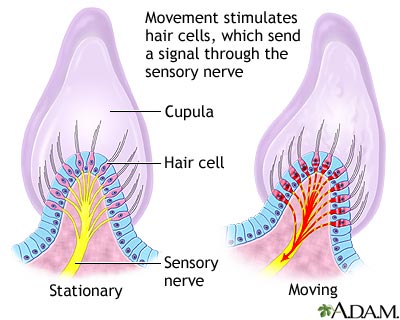
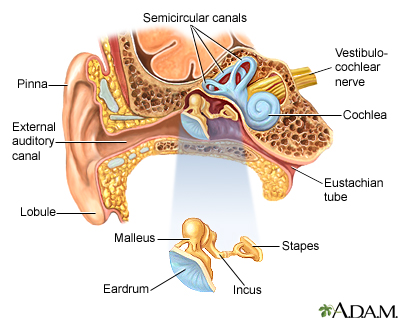
Peripheral vertigo is due to a problem in the part of the inner ear that controls balance. These areas are called the vestibular labyrinth, or semicircular canals. The problem may also involve the vestibular nerve. This is the nerve between the inner ear and the brain stem.
Peripheral vertigo may be caused by:
- Benign positional vertigo (benign paroxysmal positional vertigo, also known as BPPV)
- Certain medicines, such as aminoglycoside antibiotics, cisplatin, diuretics, or salicylates, which are toxic to the inner ear structures
- Injury (such as head injury)
- Inflammation of the vestibular nerve (neuronitis)
- Irritation and swelling of the inner ear (labyrinthitis)
- Meniere disease
- Pressure on the vestibular nerve, usually from a noncancerous tumor such as a meningioma or schwannoma
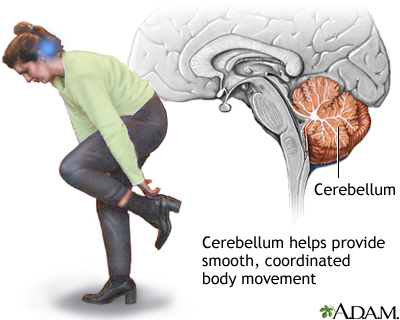
Central vertigo is due to a problem in the brain, usually in the brain stem or the back part of the brain (cerebellum).
Central vertigo may be caused by:
- Blood vessel disease
- Certain drugs, such as anticonvulsants, aspirin, and alcohol
- Multiple sclerosis
- Seizures (rarely)
- Stroke
- Tumors (cancerous or noncancerous)
- Vestibular migraine, a type of migraine headache
Symptoms
The main symptom is a sensation that you or the room is moving or spinning. The spinning sensation may cause nausea and vomiting.
Depending on the cause, other symptoms can include:
- Problem focusing the eyes
- Dizziness
- Hearing loss in one or both ears
- Loss of balance (may cause falls)
- Ringing in the ears
- Nausea and vomiting, leading to loss of body fluids
If you have vertigo due to problems in the brain (central vertigo), you may have other symptoms, including:
- Difficulty swallowing
- Double vision
- Eye movement problems
- Facial paralysis
- Slurred speech
- Weakness of the limbs
Exams and Tests
Examination by the health care provider may show:
- Problems walking due to loss of balance
- Eye movement problems or involuntary eye movements (nystagmus)
- Hearing loss
- Lack of coordination and balance
- Weakness
Tests that may be done include:
- Blood tests
- Brainstem auditory evoked potential studies
- Caloric stimulation
- Electroencephalogram (EEG)
- Electronystagmography
- Head CT
- Lumbar puncture
- MRI scan of head and MRA scan of blood vessels of the brain
- Walking (gait) testing
The provider may perform certain head movements on you, such as the head-thrust test. These tests help tell the difference between central and peripheral vertigo.
Treatment
The cause of any brain disorder causing vertigo should be identified and treated when possible.
To help resolve symptoms of benign positional vertigo, the provider may perform the Epley maneuver on you. This involves placing your head in different positions to help reset the balance organ.
You may be prescribed medicines to treat symptoms of peripheral vertigo, such as nausea and vomiting.
Physical therapy may help improve balance problems. You'll be taught exercises to restore your sense of balance. Exercises can also strengthen your muscles to help prevent falls.
To prevent worsening of symptoms during an episode of vertigo, try the following:
- Keep still. Sit or lie down when symptoms occur.
- Gradually resume activity.
- Avoid sudden position changes.
- Do not try to read when symptoms occur.
- Avoid bright lights.
You may need help walking when symptoms occur. Avoid hazardous activities such as driving, operating heavy machinery, and climbing until 1 week after symptoms have disappeared.
Other treatment depends on the cause of the vertigo. Surgery, including microvascular decompression, may be suggested in some cases.
Possible Complications
Vertigo can interfere with driving, work, and lifestyle. It can also cause falls, which can lead to many injuries, including hip fractures.
When to Contact a Medical Professional
Contact your provider for an appointment if you have vertigo that does not go away or interferes with your daily activities. If you have never had vertigo or if you have vertigo with other symptoms (such as double vision, slurred speech, or loss of coordination), call 911 or the local emergency number.
Related Information
DizzinessBenign positional vertigo
Meniere disease
Labyrinthitis
Multiple sclerosis
Broken bone
References
Bhattacharyya N, Gubbels SP, Schwartz SR, et al. Clinical practice guideline: benign paroxysmal positional vertigo (update). Otolaryngol Head Neck Surg. 2017;156(3_suppl):S1-S47. PMID: 28248609 www.pubmed.ncbi.nlm.nih.gov/28248609.
Chang AK. Dizziness and vertigo. In: Walls RM, Hockberger RS, Gausche-Hill M, eds. Rosen's Emergency Medicine: Concepts and Clinical Practice. 9th ed. Philadelphia, PA: Elsevier; 2018:chap 16.
Crane BT, Minor LB. Peripheral vestibular disorders. In: Flint PW, Haughey BH, Francis HW, et al, eds. Cummings Otolaryngology: Head and Neck Surgery. 7th ed. Philadelphia, PA: Elsevier; 2021:chap 167.
Kerber KA, Baloh RW. Neuro-otology: diagnosis and management of neuro-otoligical disorders. In: Jankovic J, Mazziotta JC, Pomeroy SL, Newman NJ, eds. Bradley's and Daroff's Neurology in Clinical Practice. 8th ed. Philadelphia, PA: Elsevier; 2022:chap 22.
BACK TO TOPReview Date: 11/9/2021
Reviewed By: Joseph V. Campellone, MD, Department of Neurology, Cooper Medical School at Rowan University, Camden, NJ. Review provided by VeriMed Healthcare Network. Also reviewed by David Zieve, MD, MHA, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.
 | A.D.A.M., Inc. is accredited by URAC, for Health Content Provider (www.urac.org). URAC's accreditation program is an independent audit to verify that A.D.A.M. follows rigorous standards of quality and accountability. A.D.A.M. is among the first to achieve this important distinction for online health information and services. Learn more about A.D.A.M.'s editorial policy, editorial process and privacy policy. A.D.A.M. is also a founding member of Hi-Ethics. This site complies with the HONcode standard for trustworthy health information: verify here. |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. © 1997- 2023 A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited.
