Health Library
Hepatitis
Hepatitis is swelling and inflammation of the liver.
Images
I Would Like to Learn About:
Causes
Hepatitis can be caused by:
- Immune cells in the body attacking the liver
- Infections from viruses (such as hepatitis A, hepatitis B, or hepatitis C), bacteria, or parasites
- Liver damage from alcohol or poison
- Medicines, such as an overdose of acetaminophen
- Fatty liver
Liver disease can also be caused by inherited disorders such as cystic fibrosis or hemochromatosis, a condition that involves having too much iron in your body.
Other causes include Wilson disease, a disorder in which the body retains too much copper and ingestion of toxic mushrooms.
Symptoms
Hepatitis may start and get better quickly. It may also become a long-term condition. In some cases, hepatitis may lead to liver damage, liver failure, cirrhosis, liver cancer or even death.
There are several factors that can affect how severe the condition is. These may include the cause of the liver damage and any illnesses you have. Hepatitis A, for example, is most often short-term and does not lead to chronic liver problems.
The symptoms of hepatitis include:
- Pain or bloating in the belly area
- Dark urine and pale or clay-colored stools
- Fatigue
- Low grade fever
- Itching
- Jaundice (yellowing of the skin or eyes)
- Loss of appetite
- Nausea and vomiting
- Weight loss
You may not have symptoms when first infected with hepatitis B or C. You can still develop liver failure later. If you have any risk factors for either type of hepatitis, you should be tested often.
Exams and Tests
You will have a physical exam to look for:
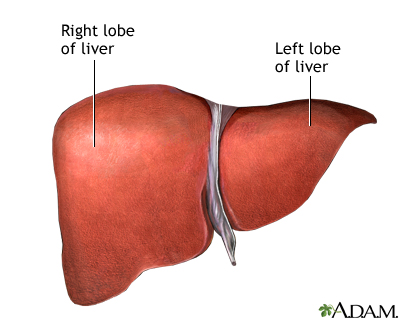
- Enlarged and tender liver
- Fluid in the abdomen (ascites)
- Yellowing of the skin
You may have lab tests to diagnose and monitor your condition, including:
- Ultrasound of the abdomen
- Autoimmune blood markers
- Blood tests to diagnose Hepatitis A, B, or C
- Liver function tests
- Liver biopsy to check for liver damage (may be needed in some cases)
- Paracentesis (if fluid is in your abdomen)
Treatment
Your health care provider will talk to you about treatment options. Treatments will vary, depending on the cause of your liver disease. You may need to eat a high-calorie diet if you are losing weight.
Support Groups
More information and support for people with hepatitis and their families can be found by joining a support group. Ask your provider about liver disease resources and support groups in your area.
Outlook (Prognosis)
The outlook for hepatitis will depend on what is causing the liver damage.
Possible Complications
Complications may include:
- Permanent liver damage, called cirrhosis
- Liver failure
- Liver cancer
When to Contact a Medical Professional
Seek care immediately if you:
- Have symptoms from too much acetaminophen or other medicines. You may need to have your stomach pumped
- Vomit blood
- Have bloody or tarry stools
- Are confused or delirious
Contact your provider if:
- You have any symptoms of hepatitis or believe that you have been exposed to hepatitis A, B, or C.
- You cannot keep food down due to excessive vomiting. You may need to receive nutrition through a vein (intravenously).
- You feel sick and have travelled to Asia, Africa, South America, or Central America.
Prevention
Talk to your provider about having a vaccine to prevent hepatitis A and hepatitis B.
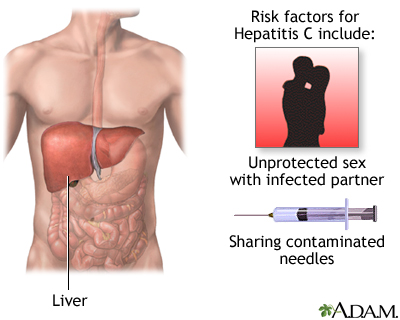
Steps for preventing the spread of hepatitis B and C from one person to another include:
- Avoid sharing personal items, such as razors or toothbrushes.
- DO NOT share drug needles or other drug equipment (such as straws for snorting drugs).
- Clean blood spills with a mixture of 1 part household bleach to 9 parts water.
- DO NOT get tattoos or body piercings with instruments that have not been cleaned properly.
To reduce your risk for spreading or catching hepatitis A:
- Always wash your hands well after using the restroom, and when you come in contact with an infected person's blood, stools, or other bodily fluid.
- Avoid unclean food and water.
Related Information
Hepatitis AHepatitis B
Hepatitis C
Autoimmune hepatitis
Drug-induced liver injury
Alcoholic liver disease
Peritonitis - spontaneous bacterial
References
Centers for Disease Control and Prevention website. Guidelines for viral hepatitis surveillance and case management. www.cdc.gov/hepatitis/statistics/surveillanceguidelines.htm. Updated May 31, 2015. Accessed April 26. 2022.
Czaja AJ. Autoimmune hepatitis. In: Feldman M, Friedman LS, Brandt LJ, eds. Sleisenger and Fordtran's Gastrointestinal and Liver Disease. 11th ed. Philadelphia, PA: Elsevier; 2021:chap 90.
Pawlotsky J-M. Chronic viral and autoimmune hepatitis. In: Goldman L, Schafer AI, eds. Goldman-Cecil Medicine. 26th ed. Philadelphia, PA: Elsevier; 2020:chap 140.
Takyar V, Ghany MG. Hepatitis A, B, D, and E. In: Kellerman RD, Rakel DP, eds. Conn's Current Therapy 2022. Philadelphia, PA: Elsevier; 2022:223-229.
Young J-A H, Ustun C. Infections in recipients of hematopoietic stem cell transplants. In: Bennett JE, Dolin R, Blaser MJ, eds. Mandell, Douglas, and Bennett's Principles and Practice of Infectious Diseases. 9th ed. Philadelphia, PA: Elsevier; 2020:chap 307.
BACK TO TOPReview Date: 2/7/2022
Reviewed By: Michael M. Phillips, MD, Emeritus Professor of Medicine, The George Washington University School of Medicine, Washington, DC. Also reviewed by David Zieve, MD, MHA, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.
 | A.D.A.M., Inc. is accredited by URAC, for Health Content Provider (www.urac.org). URAC's accreditation program is an independent audit to verify that A.D.A.M. follows rigorous standards of quality and accountability. A.D.A.M. is among the first to achieve this important distinction for online health information and services. Learn more about A.D.A.M.'s editorial policy, editorial process and privacy policy. A.D.A.M. is also a founding member of Hi-Ethics. This site complies with the HONcode standard for trustworthy health information: verify here. |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. © 1997- 2022 A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited.
