Health Library
Aneurysm
Aneurysm - splenic artery; Aneurysm - popliteal artery; Aneurysm - mesenteric artery
An aneurysm is an abnormal widening or ballooning of a part of an artery due to weakness in the wall of the blood vessel.
Images
I Would Like to Learn About:
Causes
It is not clear exactly what causes aneurysms. Some aneurysms are present at birth (congenital). Defects in some parts of the artery wall may be a cause.
Common locations for aneurysms include:
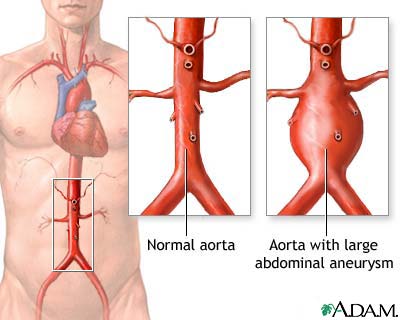
- Major artery from the heart such as the thoracic or abdominal aorta
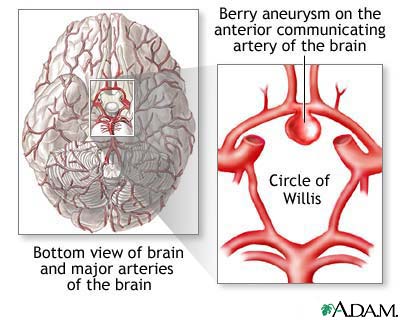
- Brain (cerebral aneurysm)
- Behind the knee (popliteal artery aneurysm)
- Intestine (mesenteric artery aneurysm)
- Artery in the spleen (splenic artery aneurysm)
Certain factors or conditions may increase the risk for aneurysms including:
- High blood pressure (thoracic, abdominal and cerebral aneurysms)
- High cholesterol
- Cigarette smoking
- Illicit drug use (cocaine, amphetamines)
- Pregnancy (often linked to splenic artery aneurysms)
- Family history (sibling, parent, or child)
Inherited disorders that may increase the risk include:
- Fibromuscular dysplasia (abnormal cell growth in artery walls)
- Polycystic kidney disease
- Coarctation of the aorta
- Cerebral arteriovenous malformation (AVM)
Symptoms
The symptoms depend on where the aneurysm is located. If the aneurysm occurs near the body's surface, pain and swelling with a throbbing lump is often seen.
Aneurysms in the body or brain often cause no symptoms. Aneurysms in the brain may expand without breaking open (rupturing). The expanded aneurysm may press on nerves and cause double vision, dizziness, or headaches. Some aneurysms may cause ringing in the ears.
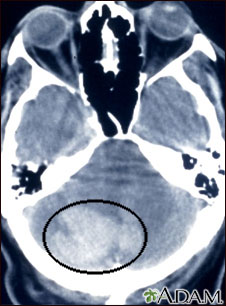
If an aneurysm ruptures, pain, low blood pressure, a rapid heart rate, and lightheadedness may occur. When a brain aneurysm ruptures, there is a sudden severe headache that some people say is the "worst headache of my life." The risk of neurologic injury, coma, or death after a rupture is high.
Exams and Tests
The health care provider will perform a physical exam.
Tests used to diagnose an aneurysm include:
- CT scan
- CT angiogram
- MRI
- MRA
- Ultrasound
- Angiogram
Treatment
Treatment depends on the size and location of the aneurysm. Your provider may only recommend regular checkups to see if the aneurysm is growing.
Surgery may be done. The type of surgery that is done and when you need it depend on your symptoms and the size and type of aneurysm.
Surgery may involve a large (open) surgical cut. Sometimes, a procedure called endovascular embolization is done. Coils or stents of metal are inserted into a brain aneurysm to make the aneurysm clot. This reduces the risk for rupture while keeping the artery open. Other brain aneurysms may need to have a clip placed on them to close them off and prevent a rupture.
Aneurysms of the aorta may be reinforced with surgery to strengthen the blood vessel wall.
When to Contact a Medical Professional
Call your provider if you develop a lump on your body, whether or not it is painful and throbbing.
Go to the emergency room or call 911 or the local emergency number if you have:
- Pain in your belly or back that is very bad or does not go away
- A sudden or severe headache, especially if you also have nausea, vomiting, seizures, or any other nervous system symptom
If you are diagnosed with an aneurysm that has not bled, you will need to have regular testing to detect if it increases in size.
Prevention
Controlling high blood pressure may help prevent many aneurysms. Follow a healthy diet, get regular exercise, and keep your cholesterol at a healthy level to help prevent aneurysms or their complications.
Do not smoke. If you do smoke, quitting will lower your risk for an aneurysm.
Related Information
Abdominal aortic aneurysmThoracic aortic aneurysm
Aneurysm in the brain
References
Lawrence PF, Rigberg DA. Arterial aneurysms: etiology, epidemiology, and natural history. In: Sidawy AN, Perler BA, eds. Rutherford's Vascular Surgery and Endovascular Therapy. 10th ed. Philadelphia, PA: Elsevier; 2023:chap 71.
Lee JJ, Mambelli DD, Britz GW. Surgical approaches to intracranial aneurysms. In: Winn HR, ed. Youmans and Winn Neurological Surgery. 8th ed. Philadelphia, PA: Elsevier; 2023:chap 435.
Mills JL, Zachary Sr, Pallister S. Peripheral arterial disease. In: Townsend CM Jr, Beauchamp RD, Evers BM, Mattox KL, eds. Sabiston Textbook of Surgery. 21st ed. St Louis, MO: Elsevier; 2022:chap 63.
BACK TO TOPReview Date: 5/2/2022
Reviewed By: Amit M. Shelat, DO, FACP, FAAN, Attending Neurologist and Assistant Professor of Clinical Neurology, Renaissance School of Medicine at Stony Brook University, Stony Brook, NY. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.
 | A.D.A.M., Inc. is accredited by URAC, for Health Content Provider (www.urac.org). URAC's accreditation program is an independent audit to verify that A.D.A.M. follows rigorous standards of quality and accountability. A.D.A.M. is among the first to achieve this important distinction for online health information and services. Learn more about A.D.A.M.'s editorial policy, editorial process and privacy policy. A.D.A.M. is also a founding member of Hi-Ethics. This site complies with the HONcode standard for trustworthy health information: verify here. |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. © 1997- 2022 A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited.
