Health Library
Intestinal obstruction and Ileus
Paralytic ileus; Intestinal volvulus; Bowel obstruction; Ileus; Pseudo-obstruction - intestinal; Colonic ileus; Small bowel obstruction
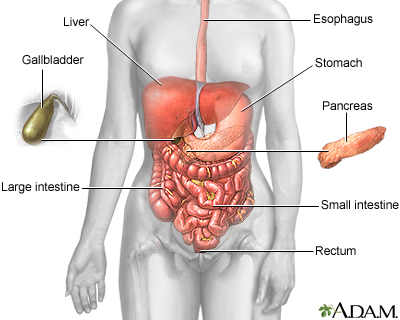
Intestinal obstruction is a partial or complete blockage of the bowel. The contents of the intestine cannot pass through it.
Images

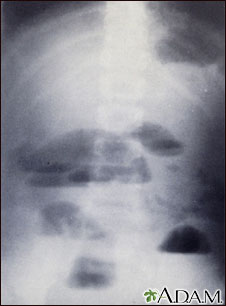
Presentation
I Would Like to Learn About:
Causes
Obstruction of the bowel may be due to:
- A mechanical cause, which means something is blocking the bowel
- Ileus, a condition in which the bowel does not work correctly, but there is no structural problem causing it
Paralytic ileus, also called pseudo-obstruction, is one of the major causes of intestinal obstruction in infants and children. Causes of paralytic ileus may include:
- Bacteria or viruses that cause intestinal infections (gastroenteritis)
- Chemical, electrolyte, or mineral imbalances (such as decreased blood potassium level)
- Abdominal surgery
- Decreased blood supply to the intestines
- Infections inside the abdomen, such as appendicitis
- Kidney or lung disease
- Use of certain medicines, especially narcotics
Mechanical causes of intestinal obstruction may include:
- Adhesions or scar tissue that form after surgery
- Foreign bodies (objects that are swallowed and block the intestines)
- Gallstones (rare)
- Hernias
- Impacted stool
- Intussusception (telescoping of one segment of bowel into another)
- Tumors blocking the intestines
- Volvulus (twisted intestine)
Symptoms
Symptoms may include:
- Abdominal swelling (distention)
- Abdominal fullness, gas
- Abdominal pain and cramping
- Breath odor
- Constipation
- Diarrhea
- Inability to pass gas
- Vomiting
Exams and Tests
During a physical exam, the health care provider may find bloating, tenderness, or hernias in the abdomen.
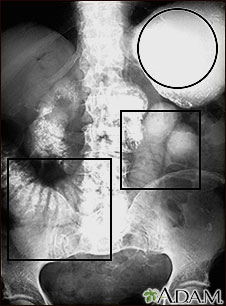
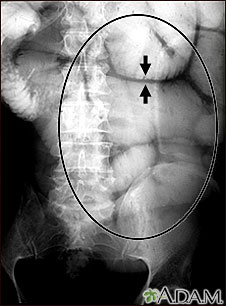
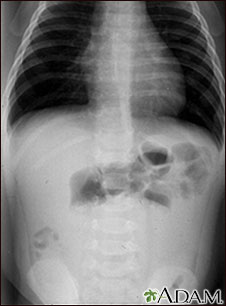
Tests that show obstruction include:
- Abdominal CT scan
- Abdominal x-ray
- Barium enema
- Upper GI and small bowel series
Treatment
Treatment involves placing a tube through the nose into the stomach or intestine. This is to help relieve abdominal swelling (distention) and vomiting. Volvulus of the large bowel may be treated by passing a tube into the rectum.
Surgery may be needed to relieve the obstruction if the tube does not relieve the symptoms. It may also be needed if there are signs of tissue death.
Outlook (Prognosis)
The outcome depends on the cause of the blockage. Most of the time, the cause is successfully treated.
Possible Complications
Complications may include or may lead to:
- Electrolyte (blood chemical and mineral) imbalances
- Dehydration
- Hole (perforation) in the intestine
- Infection
- Jaundice (yellowing of the skin and eyes)
If the obstruction blocks the blood supply to the intestine, it may cause infection and tissue death (gangrene). Risks for tissue death are related to the cause of the blockage and how long it has been present. Hernias, volvulus, and intussusception carry a higher gangrene risk.
In a newborn, paralytic ileus that destroys the bowel wall (necrotizing enterocolitis) is a life-threatening condition. It may lead to blood and lung infections.
When to Contact a Medical Professional
Contact your provider if you:
- Cannot pass stool or gas
- Have a swollen abdomen (distention) that does not go away
- Keep vomiting
- Have unexplained abdominal pain that does not go away
Prevention
Prevention depends on the cause. Treating conditions, such as tumors and hernias that can lead to a blockage, may reduce your risk.
Some causes of obstruction cannot be prevented.
Related Information
PeritonitisAbdomen - swollen
Abdominal sounds
Hernia
Gallstones
Tumor
Intussusception – children
Crohn disease
Intestinal obstruction repair
Clear liquid diet
Full liquid diet
Large bowel resection - discharge
Small bowel resection - discharge
Total colectomy or proctocolectomy - discharge
References
Galandiuk S, Netz U, Morpurgo S, et al. Colon and rectum. In: Townsend CM Jr, Beauchamp RD, Evers BM, Mattox KL, eds. Sabiston Textbook of Surgery. 21st ed. Philadelphia, PA: Elsevier; 2022:chap 52.
Gan T, Evers BM. Small intestine. In: Townsend CM Jr, Beauchamp RD, Evers BM, Mattox KL, eds. Sabiston Textbook of Surgery. 21st ed. Philadelphia, PA: Elsevier; 2022:chap 50.
Mustain WC, Turnage RH. Intestinal obstruction. In: Feldman M, Friedman LS, Brandt LJ, eds. Sleisenger and Fordtran's Gastrointestinal and Liver Disease. 11th ed. Philadelphia, PA: Elsevier; 2021:chap 123.
BACK TO TOPReview Date: 5/4/2022
Reviewed By: Michael M. Phillips, MD, Emeritus Professor of Medicine, The George Washington University School of Medicine, Washington, DC. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.
 | A.D.A.M., Inc. is accredited by URAC, for Health Content Provider (www.urac.org). URAC's accreditation program is an independent audit to verify that A.D.A.M. follows rigorous standards of quality and accountability. A.D.A.M. is among the first to achieve this important distinction for online health information and services. Learn more about A.D.A.M.'s editorial policy, editorial process and privacy policy. A.D.A.M. is also a founding member of Hi-Ethics. This site complies with the HONcode standard for trustworthy health information: verify here. |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. © 1997- 2022 A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited.
