Pseudomembranous colitis
Antibiotic-associated colitis; Colitis - pseudomembranous; Necrotizing colitis; C difficile - pseudomembranous
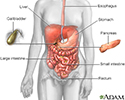
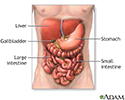
Pseudomembranous colitis refers to swelling or inflammation of the large intestine (colon) due to an overgrowth of Clostridioides difficile (C difficile) bacteria.
This infection is a common cause of diarrhea after antibiotic use. Not all cases of diarrhea associated with antibiotic use are due to C difficile or will progress to pseudomembranous colitis.
Causes
The C difficile bacteria normally lives in the intestine. However, too much of these bacteria may grow when you take antibiotics. The bacteria give off a strong toxin that causes inflammation and bleeding in the lining of the colon.
Any antibiotic can cause this condition. The drugs responsible for the problem most of the time are ampicillin, clindamycin, fluoroquinolones, and cephalosporins.
Health care providers in the hospital may pass this bacteria from one patient to another.
Pseudomembranous colitis is uncommon in children, and rare in infants. It is most often seen in people who are in the hospital. However, it is becoming more common in people who take antibiotics and are not in a hospital.
Risk factors include:
- Older age
- Antibiotic use
- Use of medicines that weaken the immune system (such as chemotherapy medicines)
- Recent surgery
- History of pseudomembranous colitis
- History of ulcerative colitis and Crohn disease
Symptoms
Symptoms include:
- Abdominal cramps (mild to severe)
- Bloody stools
- Fever
- Urge to have a bowel movement
- Watery diarrhea (often 5 to 10 times per day)
Exams and Tests
The following tests may be done:
- Colonoscopy or flexible sigmoidoscopy
- Immunoassay for C difficile toxin in the stool
- Polymerase chain reaction (PCR) for C difficile toxin in the stool
Treatment
The antibiotic or other medicine causing the condition should be stopped. Metronidazole, vancomycin, or fidaxomicin are most often used to treat the problem, but other medicines may also be used.
Electrolyte solutions or fluids given through a vein may be needed to treat dehydration due to diarrhea. In rare cases, surgery is needed to treat infections that get worse or do not respond to antibiotics.
Long term antibiotics may be needed if the C difficile infection returns. A treatment called fecal microbiota transplant ("stool transplant") has also been effective for infections that come back.
Your provider may also suggest that you take probiotics if the infection returns.
Outlook (Prognosis)
The outlook is good in most cases, if there are no complications. However, up to 1 in 5 infections may return and need more treatment.
Possible Complications
Complications may include:
- Dehydration with electrolyte imbalance
- Perforation of (hole through) the colon
- Toxic megacolon
- Death
When to Contact a Medical Professional
Contact your provider if you have the following symptoms:
- Any bloody stools (especially after taking antibiotics)
- Five or more episodes of diarrhea per day for more than 1 to 2 days
- Severe abdominal pain
- Signs of dehydration
Prevention
People who have had pseudomembranous colitis should tell their providers before taking antibiotics again. It is also very important to wash hands well to prevent passing the germ to other people. Alcohol sanitizers do not always work on C difficile.
References
Gerding DN, Johnson S. Clostridial infections. In: Goldman L, Schafer AI, eds. Goldman-Cecil Medicine. 26th ed. Philadelphia, PA: Elsevier; 2020:chap 280.
Gerding DN, Young VB. Donskey CJ. Clostridiodes difficile (formerly Clostridium difficle) infection. In: Bennett JE, Dolin R, Blaser MJ, eds. Mandell, Douglas, and Bennett's Principles and Practice of Infectious Diseases. 9th ed. Philadelphia, PA: Elsevier; 2020:chap 243.
Johnson S, Lavergne V, Skinner AM, et al. Clinical practice guideline by the Infectious Diseases Society of America (IDSA) and Society for Healthcare Epidemiology of America (SHEA): 2021 focused update guidelines on management of clostridioides difficile infection in adults. Clin Infect Dis. 2021; 73(5):e1029-e1044. PMID: 34164674 pubmed.ncbi.nlm.nih.gov/34164674/.
Kelly CP, Khanna S. Antibiotic-associated diarrhea and clostridioides difficile infection. In: Feldman M, Friedman LS, Brandt LJ, eds. Sleisenger and Fordtran's Gastrointestinal and Liver Disease. 11th ed. Philadelphia, PA: Elsevier; 2021:chap 112.
Review Date: 5/4/2022
Reviewed By: Michael M. Phillips, MD, Emeritus Professor of Medicine, The George Washington University School of Medicine, Washington, DC. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.