Collateral ligament (CL) injury - aftercare
Medial collateral ligament injury - aftercare; MCL injury - aftercare; Lateral collateral ligament injury - aftercare; LCL injury - aftercare; Knee injury - collateral ligament
A ligament is a band of tissue that connects a bone to another bone. The collateral ligaments of the knee are located on the outside part of your knee joint. They help connect the bones of your upper and lower leg, around your knee joint.
- The lateral collateral ligament (LCL) runs on the outer side of your knee.
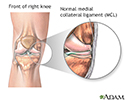
- The medial collateral ligament (MCL) runs along the inside of your knee.
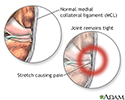
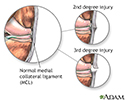
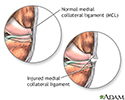
A collateral ligament injury occurs when the ligaments are stretched or torn. A partial tear occurs when only part of the ligament is torn. A complete tear occurs when the entire ligament is torn into two pieces.
More About Your Injury
The collateral ligaments help keep your knee stable. They help keep your leg bones in place and keep your knee from moving too far sideways.
A collateral ligament injury can occur if you get hit very hard on the inside or outside of your knee, or when you have a twisting injury.
Skiers and people who play basketball, football, or soccer are more likely to have this type of injury.
What to Expect
With a collateral ligament injury, you may notice:
- A loud pop when the injury occurs
- Your knee is unstable and can shift side to side as if it "gives way"
- Locking or catching of the knee with movement
- Knee swelling
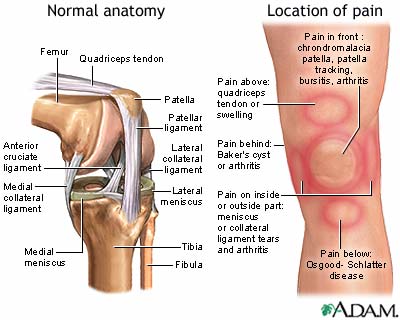
- Knee pain along the inside or outside of your knee
After examining your knee, the doctor may order these imaging tests:
- X-rays to check for damage to the bones in your knee.
- An MRI of the knee. An MRI machine takes special pictures of the tissues inside your knee. The pictures will show whether these tissues have been stretched or torn.
If you have a collateral ligament injury, you may need:
- Crutches to walk until the swelling and pain get better
- A brace to support and stabilize your knee
- Physical therapy to help improve joint motion and leg strength
- Surgery to repair the collateral ligament or other associated injuries
Most people do not need surgery for an MCL injury. However, you may need surgery if your LCL is injured or if your injuries are severe and involve other ligaments in your knee.
Self-care at Home
Follow R.I.C.E. to help reduce pain and swelling:
- Rest your leg. Avoid putting weight on it.
- Ice your knee for 20 minutes at a time, 3 to 4 times a day.
- Compress the area by wrapping it with an elastic bandage or compression wrap.
- Elevate your leg by raising it above the level of your heart.
You can use ibuprofen (Advil, Motrin), or naproxen (Aleve, Naprosyn) to reduce pain and swelling. Acetaminophen (Tylenol) helps with pain, but not swelling. You can buy these pain medicines at the store.
- Talk with your doctor before using these medicines if you have heart disease, high blood pressure, kidney disease, or have had stomach ulcers or internal bleeding in the past.
- Do not take more than the amount recommended on the bottle or by your doctor.
Activity
You should not put all of your weight on your leg if it hurts. You should check with your doctor about how much weight you should put on your leg. Rest and self-care may be enough to allow the tear to heal. You should use crutches to protect the injured ligament.
You may need to work with a physical therapist (PT) to regain knee and leg strength. The PT will teach you exercises to strengthen the muscles, ligaments, and tendons around your knee.
As your knee heals, you can return to normal activities and maybe play sports again.
When to Call the Doctor
Call your doctor if:
- You have increased swelling or pain
- Self-care does not seem to help
- You lose feeling in your foot
- Your foot or leg feels cold or changes color
If you have surgery, call the doctor if you have:
- A fever of 100°F (38°C) or higher
- Drainage from the incisions
- Bleeding that won't stop
References
Lamplot JD, Bogunovic L, Wright RW. Revision anterior cruciate ligament injuries. In: Miller MD, Thompson SR, eds. DeLee, Drez, & Miller's Orthopaedic Sports Medicine. 5th ed. Philadelphia, PA: Elsevier; 2020:chap 99.
Lento P, Marshall B, Akuthota V. Collateral ligament sprain. In: Frontera WR, Silver JK, Rizzo TD, Jr, eds. Essentials of Physical Medicine and Rehabilitation. 4th ed. Philadelphia, PA: Elsevier; 2019:chap 66.
Miller RH, Azar FM. Knee injuries. In: Azar FM, Beaty JH eds. Campbell's Operative Orthopaedics. 14th ed. Philadelphia, PA: Elsevier; 2021:chap 45.
Yonz MC, Wilson BF, Blake MH, Johnson DL. Medial collateral ligament and posterior medial corner injuries. In: Miller MD, Thompson SR, eds. DeLee, Drez, & Miller's Orthopaedic Sports Medicine. 5th ed. Philadelphia, PA: Elsevier; 2020:chap 101.
Medial collateral ligament - illustration
Medial collateral ligament
illustration
Knee pain - illustration
Knee pain
illustration
Medial collateral ligament pain - illustration
Medial collateral ligament pain
illustration
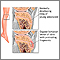
Medial collateral ligament injury - illustration
Medial collateral ligament injury
illustration
Torn medial collateral ligament - illustration
Torn medial collateral ligament
illustration
Medial collateral ligament - illustration
Medial collateral ligament
illustration
Knee pain - illustration
Knee pain
illustration
Medial collateral ligament pain - illustration
Medial collateral ligament pain
illustration
Medial collateral ligament injury - illustration
Medial collateral ligament injury
illustration
Torn medial collateral ligament - illustration
Torn medial collateral ligament
illustration
Review Date: 6/13/2021
Reviewed By: C. Benjamin Ma, MD, Professor, Chief, Sports Medicine and Shoulder Service, UCSF Department of Orthopaedic Surgery, San Francisco, CA. Also reviewed by David Zieve, MD, MHA, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.