Anti-reflux surgery - discharge
Fundoplication - discharge; Nissen fundoplication - discharge; Belsey (Mark IV) fundoplication - discharge; Toupet fundoplication - discharge; Thal fundoplication - discharge; Hiatal hernia repair - discharge; Endoluminal fundoplication - discharge; GERD - fundoplication discharge; Gastroesophageal reflux disease - fundoplication discharge
You had surgery to treat your gastroesophageal reflux disease (GERD). GERD is a condition that causes food or liquid to come up from your stomach into your esophagus (the tube that carries food from your mouth to your stomach).
Now that you're going home, be sure to follow your surgeon's instructions on how to take care of yourself.
When You're in the Hospital
If you had a hiatal hernia, it was repaired. A hiatal hernia develops when the natural opening in your diaphragm is too large. Your diaphragm is the muscle between your chest and belly. Your stomach may bulge through this large hole into your chest. This bulging is called a hiatal hernia. It may make GERD symptoms worse.
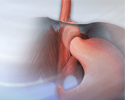
Your surgeon also wrapped the upper part of your stomach around the end of your esophagus to create pressure at the end of your esophagus. This pressure helps prevent stomach acid and food from flowing back up.
Your surgery was done by making a large incision in your upper belly (open surgery) or with a small incision using a laparoscope (a thin tube with a tiny camera on the end).
What to Expect at Home
Most people go back to work 2 to 3 weeks after laparoscopic surgery and 4 to 6 weeks after open surgery.
You may have a feeling of tightness when you swallow for 6 to 8 weeks. This is from the swelling inside your esophagus. You may also have some bloating.
Self-care
When you return home, you will be drinking a clear liquid diet for 2 weeks. You will be on a full liquid diet for about 2 weeks after that, and then a soft-food diet.
On the liquid diet:
- Start off with small amounts of liquid, about 1 cup (237 mL) at a time. Sip. Do not gulp. Drink liquids often during the day after surgery.
- Avoid cold liquids.
- Do not drink carbonated beverages.
- Do not drink through straws (they can bring air into your stomach).
- Crush pills and take them with liquids for the first month after surgery.
When you are eating solid foods again, chew well. Do not eat cold foods. Do not eat foods that clump together, such as rice or bread. Eat small amounts of food several times a day instead of three big meals.
Your surgeon will give you a prescription for pain medicine. Get it filled when you go home so you have it when you need it. Take your pain medicine before your pain becomes too severe.
- If you have gas pains, try walking around to ease them.
- Do not drive, operate any machinery, or drink alcohol when you are taking narcotic pain medicine. This medicine can make you very drowsy and driving or using machinery is not safe.
Walk several times a day. Do not lift anything heavier than 10 pounds (about a gallon of milk; 4.5 kg). Do not do any pushing or pulling. Slowly increase how much you do around the house. Your surgeon will tell you when you can increase your activity and return to work.
Wound Care
Take care of your wound (incision):
- If sutures (stitches), staples, or glue were used to close your skin, you may remove the wound dressings (bandages) and take a shower the day after surgery.
- If tape strips were used to close your skin, cover the wounds with plastic wrap before showering for the first week. Tape the edges of the plastic carefully to keep water out. Do not try to wash the strips off. They will fall off on their own after about a week.
- Do not soak in a bathtub or hot tub, or go swimming, until your doctor tells you it is OK.
When to Call the Doctor
Contact your health care provider if you have any of the following:
- Temperature of 101°F (38.3°C) or higher
- Incisions are bleeding, red, warm to the touch, or have a thick, yellow, green, or milky drainage
- Belly swells or hurts
- Nausea or vomiting for more than 24 hours
- Problems swallowing that keep you from eating
- Problems swallowing that do not go away after 2 or 3 weeks
- Pain medicine is not helping your pain
- Trouble breathing
- Cough that does not go away
- Can't drink or eat
- Skin or the white part of your eyes turns yellow
References
Katz PO, Dunbar KB, Schnoll-Sussman FH, Greer KB, Yadlapati R, Spechler SJ. ACG clinical guideline for the diagnosis and management of gastroesophageal reflux disease. Am J Gastroenterol. 2022;117(1):27-56. PMID: 34807007 pubmed.ncbi.nlm.nih.gov/34807007/.
Richter JE, Vaezi MF. Gastroesophageal reflux disease. In: Feldman M, Friedman LS, Brandt LJ, eds. Sleisenger and Fordtran's Gastrointestinal and Liver Disease. 11th ed. Philadelphia, PA: Elsevier; 2021:chap 46.
Yates RB, Oelschlager BK. Gastroesophageal reflux disease and hiatal hernia. In: Townsend CM Jr, Beauchamp RD, Evers BM, Mattox KL, eds. Sabiston Textbook of Surgery. 21st ed. St Louis, MO: Elsevier; 2022:chap 43.
Review Date: 10/1/2022
Reviewed By: Debra G. Wechter, MD, FACS, General Surgery Practice Specializing in Breast Cancer, Virginia Mason Medical Center, Seattle, WA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.